
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS
ALGORITHM FOR A WIRELESS BODY SENSOR PLATFORM
Francisco J. Rinc´on
1
, Laura Guti´errez
1
, M´onica Jim´enez
1
, V´ıctor D´ıaz
2
, Nadia Khaled
3
David Atienza
1, 4
, Marcos S´anchez-
´
Elez
1
, Joaqu´ın Recas
1
and Giovanni De Micheli
3
1
DACYA/UCM, Madrid, Spain
Depto. Salud y Rendimiento Humano/UPM, Madrid, Spain
3
LSI/EPFL, Lausanne, Switzerland
ESL/EPFL, Lausanne, Switzerland
Keywords:
Wireless Body Sensor Networks, Biomedical signal processing, Electrocardiogram.
Abstract:
Wireless Body Sensor Networks (WBSN) are poised to become a key enabling technology of personal systems
for pervasive healthcare. Recent results have however shown that the conventional approach to their design,
which consists in continuous wireless streaming of the sensed data to a central data collector, is unsustainable
in terms of network lifetime and autonomy. Furthermore, it was established that wireless data communica-
tion is responsible for most of the energy consumption. To address the energy inefficiency of conventional
WBSNs, we advocate an advanced WBSN concept where sensor nodes exploit their available, yet limited
processing and storage resources to deploy advanced embedded intelligence and processing, to reduce the
amount of wireless data communication and consequently energy consumption. More specifically, this paper
addresses the design and optimization of an automated real-time electrocardiogram (ECG) signal analysis and
cardiovascular arrhythmia diagnosis application for a prototype sensor node called Wireless 25 EEG/ECG sys-
tem. The satifactory accuracy of this on-line automated ECG-based analysis and diagnosis system is assessed
and compared to the salient off-line automated ECG analysis algorithms. More importantly, our results show
an energy consumption reduction of 80% to 100% with respect to conventional WBSNs, when our analysis
and diagnosis algorithm is used to process the sensed ECG data to extract its relevant features, which are
then wirelessly reported to the WBSN central data collector, after the node can automatically determine the
potential cardiovascular pathology without human monitoring.
1 INTRODUCTION
AND RELATED WORK
Wearable personal health systems for pervasive mon-
itoring and healthcare are widely recognized to
be a key enabling integration technology for next-
generation advanced citizen-centric eHealth delivery
solutions (Lo and Yang, 2005). Through enabling
continuous biomedical monitoring and care, they hold
the promise of improved personalization and qual-
ity of care, increased ability of prevention and early
∗
This work is partially supported by the Spanish Gov-
ernment Research Grant TIC 2005-5619 and the Integrated
Systems Center of EPFL under the project ”Performance
monitoring for professional and recreation sports using
Wireless Sensor Networks” (2007-2008).
diagnosis, and enhanced patient autonomy. Further-
more, wearable personal health systems can help the
eHealth sector realize rapid sustained market growth,
reduction of healthcare and public costs.
To provide the necessary accurate, integrated and
long-term assessment and feedback, these wearable
personal health systems must sense, acquire, moni-
tor and analyze a large number of physiological and
metabolic parameters, both during physical activity
and rest. The number as well as the nature of the pa-
rameters of interest depends on the actual biomedical
application/scenario and target population. Neverthe-
less, it is largely accepted that Wireless Body Sen-
sor Networks (WBSN) will be the underlying com-
mon architecture and technology of these personal
health systems. More specifically, the WBSN will
88
Rincón F., Gutiérrez L., Jiménez M., Díaz V., Khaled N., Atienza D., Sánchez-Élez M., Recas J. and De Micheli G. (2009).
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS ALGORITHM FOR A WIRELESS BODY SENSOR PLATAFORM.
In Proceedings of the International Conference on Biomedical Electronics and Devices, pages 88-96
DOI: 10.5220/0001549000880096
Copyright
c
SciTePress

consist of a number of sensor nodes attached to the
patient body, each sensor node potentially compris-
ing of 5 components (Lazzer et al., 2002; Culler
et al., 2004): sensors, actuators, a microprocessor,
a wireless transceiver and an energy source. Each
WBSN node ensures the accurate sensing and capture
of its target physiological data, its (pre-) processing
and wireless communication to the other nodes and
the wearable Personal Digital Assistant (PDA). This
PDA will be responsible for the storage, organization,
complementary analysis and fusion of the collected
information, its user-friendly representation, and its
dissemination to the relevant medical staff or cen-
tral monitoring service through private and/or public
wireless access networks (Lo and Yang, 2005).
State-of-the-art commercial products and experi-
mental prototypes of personal health monitoring sys-
tems merely apply on-board analog filtering to the
sampled sensed data, before it is either logged on a
bulky patient unit for off-line analysis, or wirelessly
transmitted to a remote monitoring system (Jovanov
and et al., 2005; LifeShirt, ; SmartShirt, ). The ob-
trusiveness and off-line nature of the analysis of the
first approach compromises its acceptance and appli-
cability to pervasive healthcare, whereas the second
approach is not sustainable in free-living conditions in
terms of autonomy. Indeed, current results in WBSN,
e.g., prosthesis processing (Kemere and et al., 2004)
or Electroencephalogram (EEG) / Electrocardiogram
(ECG) monitoring (L¨ofgren and et al., 2007)) indi-
cate that an unaffordable amount of energy would be
spent in the wireless communication, if no local sig-
nal processing is present and most of the acquired
data is wirelessly streamed to the PDA. Moreover,
similar conclusions can be derived from the Code-
Blue project (Project, ), which is a WBSN that targets
biomedical monitoring by including a set of devices
to collect ECG and oxigen saturation data, which can
be transmitted through a wireless network to a wide
range of receiving devices that can display the data
in real time. The conclusions of this project outline
that the largest proportion of energy is consumed in
the wireless data transmission, and requires monitor-
ing of the received data by a doctor or biomedical
specialist; thus, the WBSN nodes are not able to re-
port any physical anomaly. Therefore, we advocate
in this paper an advanced WBSN concept where sen-
sor nodes exploit their available processing and stor-
age resources to deploy advanced embedded intelli-
gence and processing, which will be optimized for
enhanced functionality and autonomy. More partic-
ularly, in this paper, we investigate the feasibility and
benefits of such an advanced WBSN for an automated
electrocardiogram (ECG) signal analysis and cardio-
vascular arrhythmia recognition application, using a
prototype sensor node called Wireless 25 EEG/ECG
system (Penders et al., 2007).
A significant amount of research effort has been
devoted to the automated analysis of ECG signals.
Some of the proposed methods are able to classify
a set of Arrhythmias depending on special correlated
characteristics of the ECG signal, for instance, using
Multicategory Support Vector Machines (Khadtare
and Sahambi, 2004). Other methods are based on
the underlying detection of the major ECG charac-
teristic waves, namely the QRS complex, P and T
waves (S¨ornmo and Laguna, 2005). As a matter of
fact, the performance of an automated ECG analy-
sis system using the second approach critically de-
pends on the reliable detection of these fiducial waves.
The most salient methods proposed for the auto-
mated detection of the ECG fiducial waves belong to
three categories: filtering or adaptive thresholding,
wavelet transform-based and (nonlinear) multiscale
transform-based (S¨ornmo and Laguna, 2005). The
latter approach was evidenced to have less noise sen-
sitivity than adaptive thresholding, and to avoid the
problem of position deviation exhibited by wavelet-
based techniques. Therefore, in this paper, we con-
sider a multiscale morphological derivative (MMD)
transform-based algorithm to realize automated ECG
characteristic wave detection.
While the retained MMD transform-based algo-
rithm was validated by simulation (Sun et al., 2005),
its translation into a robust, efficient and reliable au-
tomated diagnosis capability embedded in our wear-
able sensor node calls for the porting and (non-
straightforward) optimization of this algorithm to
adapt it to the sensor node’s limited processing re-
sources. In general, this porting and optimization
effort is key to translate the recent biomedical sig-
nal processing advances into autodiagnosis tools, and
hence to enable pervasive healthcare. As a result, the
main contributions of the paper are:
• The design of a real-time ECG-based diagnosisal-
gorithm, including a new run-time ECG signal re-
construction module, based on the off-line MMD
algorithm, and a diagnosis module able to identify
various anomalies in the cardiovascular function.
• The porting and optimization of the new real-time
ECG-based diagnosis algorithm on the Wireless
25-channel EEG/ECG sensor node platform.
• The application of the new diagnosis algorithm
for autodiagnosis on-board the sensor node to sig-
nificantly reduce the amount of data to be wire-
less transmitted, and consequently, dramatically
reduce the sensor node’s energy consumption and
extend its battery life.
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS ALGORITHM FOR A WIRELESS BODY
SENSOR PLATAFORM
89

The rest of the paper is organized as follows. In
Section 2, we overview the software and hardware
architecture of the WBSN node used in this work.
Then, in Section 3, we present the ECG-based diag-
nosis algorithm ported to our WBSN node. Next, in
Section 4, we describe the performance and energy
consumption trade-offs between node processing and
the communication tasks. Finally, in Section 5, we
summarize the main conclusions of this work.
2 WIRELESS BODY SENSOR
NODE ARCHITECTURE
As previously mentioned, this work uses as target
platform a Wireless 25-channel EEG/ECG sensor
node (Penders et al., 2007). This small sensor node
can monitor up to 25 different bio-potential signals
and transmit in real-time wirelessly the sensed infor-
mation to a data collector device. Furthermore, it
can be combined with other instances of the same
node to define complex WBSN topologies. The node
has a very elaborated hardware/software architecture,
which enables porting different types of biomedical
signal processing applications, use different hardware
components, and customize the communication stack
for various wireless communication protocols. In this
section, we summarize the main features of the har-
ware/software architecture of this node.
2.1 Hardware Architecture
The hardware architecture of the Wireless 25-channel
EEG/ECG sensor node is partitioned in three main
blocks, which relate to the three main tasks in WSNs,
namely, sensing, processing and wireless transmis-
sion of the acquired informationto a base station (e.g.,
a PC, PDA or a mobile phone).
The sensing task is performed by a 25-channel
ultra-low-power Application-Specific Integrated Cir-
cuit (ASIC) that is able to extractthe bio-potentialsig-
nals. The core of the processing part is a TI MSP430
ultra-low-power microcontroller (Lutz Bierl, 2000).
This small 16-bit microcontroller has a low active
power (0.6 nJ/instruction), as well as a a very low
stand-by power (2µW). In addition, it features a fast
wakeup from stand-by to active mode (6µs) and an
on-chip 12-bit analog-to-digital converter, suitable for
biomedical signal processing. Finally, it also includes
60kB of flash program memory and 2kB of RAM to
upload applications and store processed data from the
different sensors.
Then, the wireless communication task is carried
out using a Nordic nRF2401 transceiver (Semicon-
Radio
nRF2401
µC
MSP430
25-ch
ASIC
Radio
driver
µC
driver
ASIC
driver
MAC
TinyOSkernel
Application
Figure 1: OS-Based EEG/ECG 25-ch sensor node architec-
ture overview.
ductor, 2000), which is an ultra-low-power 2.4 GHz
communication chip. This component has a very low
power consumption, with only 10.5mA at an output
power of -5dBm and 18mA in receive mode. Also,
it includes built-in power-down modes that allow to
switch-off the radio when not used, and special trans-
mission modes to reduce the processing needed by the
microcontroller for every new packet sent or received.
Overall, this radio is a low-power solution for WBSN,
which has relatively low duty cycle rates.
2.2 Software Architecture
The software architecture of the platform follows a
layered modular approach in which each hardware
component (sensors, microcontroller and radio) is a
separate software module. This modular multi-layer
structure, depicted in Figure 1, is supported thanks
to the inclusion of TinyOS (Culler, 2006), a light
event-based operating system specially designed for
WSNs. It has been written using the nesC (Gay et al.,
2003) programming language, which is an extension
of the C language optimized for the memory restric-
tions of sensor networks. Thus, it is possible to eas-
ily port new biomedical signal processing applica-
tions using the nesC language, and to use the under-
lying hardware driver support provided by TinyOS
to access different hardware blocks in the architec-
ture. In addition, the abstraction from the hardware
blocks makes possible to modify/replacethe hardware
blocks included in each instance of the node, with-
out modifying the remaining blocks or the upper lay-
ers (communication protocols, applications, etc.). In
particular, in this research work, while a porting for
the TI MSP430 microcontroller was already available
within the TinyOS hardware support, we had to de-
velop the new drivers to support the Nordic nRF2401
radio module and the 25-channel EEG/ECG ASIC in
the operating system, to be able to use them from the
ECG-based diagnosis application layer.
BIODEVICES 2009 - International Conference on Biomedical Electronics and Devices
90

3 ECG-BASED DIAGNOSIS
ALGORITHM
The design of an ECG-based diagnosis algorithm to
detect possible cardiovascular diseases is a very com-
plex process that can be divided in two main phases.
First, a real-time detection of the characteristic waves
of ECG signals (Sun et al., 2005; Sun et al., 2002)
(e.g., complex QRS, P and T wave, etc.) is an es-
sential module for the quality of the detection of the
cardiovascular diseases; thus, we have developed a
run-time ECG wave identification module, which is
described in Section 3.1. Second, once the funda-
mental features of the input ECG signal are identi-
fied, they can be used to detect if the heart is suffer-
ing an anomalousbehaviorof the cardiovascularfunc-
tion and diagnose corresponding pathologies. This
last phase of the proposed ECG-based diagnosis al-
gorithm is described in Section 3.2.
3.1 Run-Time ECG Signal
Reconstruction
Our run-time ECG signal reconstruction phase is
based on a multiscale morphological derivative
(MMD) transform-based singularity detector (Sun
et al., 2005). This initial detector is an off-line al-
gorithm able to reliably identify the Q wave, R peak,
S wave and the onsets and offsets of the P wave and
T wave, which are fundamental blocks of any ECG
signal, as shown in Figure 2.
Although the ECG signal reconstruction using the
MMD algorithm is quite accurate (Sun et al., 2005),
the fundamental issue to directly apply for WBSN is
the fact that MMD requires as input data the com-
plete wave read from a patient during a large amount
of time, which is subsequently processed to tune the
thresholds to apply for each concrete sample. Unfor-
tunately, the memory resources of a WBSN sensor
node are very limited (only few kilobytes) to min-
imize its size and power consumption; thus, taking
into account the high sampling frequency needed for
a reliable ECG signal processing, only a few seconds
of information can be stored, which is insufficient to
accurately tune the thresholds for MMD. Moreover, if
all the data is streamed from the sensor node to a de-
vice with larger capacity (e.g., a base station) to pro-
cess them, the sensor node would run out of battery
in a short period of time, because of the elevated data
transmission rate that is needed and the high energy
consumption of the radio. As a result, WBSN require
an on-line approach for ECG signal reconstruction, in
which the complete ECG signal is processed directly
in the sensor nodes and only the relevant results are
(a)
A
B
C
D
E
F
G
H
I
J
K
(b)
(c)
Figure 2: Results obtained using the MMD detector. (a)
Original ECG input signal (b) Multiscale morphological
transform of the original signal (c) Points and waves de-
tected by the algorithm.
A=onset of the P wave, B=P peak, C=offset of the P wave, D=onset
of the Q wave, E=onset of the R wave, F=R peak, G=offset of the
R wave, H=offset of the S peak, I=onset of the T wave, J=T peak,
K=offset of the T wave.
sent to the data collector device or base station.
In the following we propose a run-time process-
ing of the ECG signal, based on a MMD transform-
based singularity detector, which can be directly ex-
ecuted in a WBSN sensor node. In the first phase of
our run-time ECG fiducial wave detection algoritm,
the received input signal is filtered for noise reduction
and baseline wander correction (S¨ornmo and Laguna,
2005). To this end, we have implemented a morpho-
logical filter on the input signal (Sun et al., 2002),
where at all instances of time during the execution,
a window of the last 300 samples are stored in a cir-
cular buffer. Hence, since the sampling frequency of
the 25-channel EEG/ECG node is 200Hz, the current
implementation of the algorithm uses the last 1.5s of
the input signal as history of processed signal.
Once each sample is filtered, the following step in
an MMD detector requires the application of a mul-
tiscale morphological transform on the filtered data
to detect the fiducial points in the original ECG sig-
nal. However, due to the scarce memory resources
in the node, the transformed signal cannot be stored
in the node; thus, the morphological transform is dy-
namically recalculated when needed during the fol-
lowing steps of the run-time algorithm. Then, the lo-
cal maxima and minima of the transformed signal can
be selected, based on some characteristics of the mor-
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS ALGORITHM FOR A WIRELESS BODY
SENSOR PLATAFORM
91

Table 1: Steps followed by the proposed run-time ECG sig-
nal reconstruction algorithm. All the operations are per-
formed over the transformed data.
1. The thresholds Th
r
and Th
f
are selected based
on an adaptive thresholding from the histogram
of the transformed signal
2. r
peak
= local minima with absolute amplitude
larger than Th
r
If r
peak
was not detected, go to 1, otherwise
continue
3. r
on
= first local maxima on the left of r
peak
with
absolute amplitude larger than Th
f
r
of f
= first local maxima on the right of r
peak
with absolute amplitude larger than Th
f
4. q
wave
= first local minima on the left of r
on
with
absolute amplitude larger than Th
f
5. s
wave
= first local minima on the right of r
of f
with absolute amplitude larger than Th
f
6. p
of f
= first local maxima on the left of q
wave
with absolute amplitude larger than Th
f
p
on
= first local maxima on the left of p
of f
with
absolute amplitude larger than Th
f
7. t
on
= first local maxima on the right of s
wave
with absolute amplitude larger than Th
f
t
of f
= first local maxima on the right of t
on
with
absolute amplitude larger than Th
f
phological trasform and a dynamic thesholding, up-
dated at run-time using a window of the last received
samples. These detected local maxima and minima
are then subsequently used to locate the characteristic
points of the wave. In this regard, since the sampling
frequency is 200Hz, the microcontroller only has 5ms
between two consecutive samples to perform all the
calculations on the data to find the local maxima and
minima. As this time interval is too short to execute
the complete detection of maxima and minima points,
we have divided the algorithm into 7 phases, which
are listed in Table 1. Each of these phases can be ex-
ecuted in the interval between two consecutive sam-
ples. Thus, when a new data is sampled, filtered and
included in the circular buffer, one of the 7 phases is
executed. For example, at the beginning of the pro-
cess, when no R peak is yet present in the considered
window, steps 1 and 2 are repeated continuously be-
tween data samples. Then, when a R peak is detected
in step 2, steps 3 to 7 are applied in sequence, such
that, each of them is used in the time slot between
two consecutive samples. After the complete identifi-
cation of the current input ECG wave is finished, the
process restarts from step 1 for the next wave.
For illustration purposes, one of the results ob-
tained using the proposed run-time ECG signal re-
construction algorithm in an input wave is depicted
in Figure 2. This figure shows three different waves,
the first one (or a) is the original ECG signal given
as an input to the algorithm. The second wave (or
b) is the original signal after applying the multiscale
morphological transform, all the points detected by
the algorithm are marked. The last one (or c) shows
the detected waves and peaks over the original signal.
This last wave illustrates where the Q wave, R peak,
S wave and the onsets and offsets of the P and T wave
are found using our run-time algorithm.
3.2 Arrhythmia Detection Phase
After processing the original ECG signal and obtain-
ing the fiducial points of the wave (Figure 2), our
diagnosis module is applied to check if the signal
presents any anomalous behavior,which may hint that
the patient is suffering a cardiovascular pathology.
The diagnosis module checks iteratively five dif-
ferent conditions based in the points detected in the
ECG signal, according to the valid ranges reported
in (Schamroth, 1971; P´erez-G´omez, 1985), namely:
1. The time from D to H must be less or equal to
0.10s.
2. The time interval from A to D must be in the range
from 0.12s to 0.20s.
3. The amplitude of J must always be positive.
4. The time from D to F must not be longer than
0.03s.
5. The QT interval rule, which establishes a relation
between the interval from D to K. This rule indi-
cates the valid interval between the heart beat rate,
and the last RR interval (i.e., the interval from the
last R peak to the current one). To find the valid
QT interval, Bazet’s formula (1) is used to calcu-
late the QT coefficient for an input signal (QTc)
as shown in Equation 1. Then, the valid values of
the QTc are reported in Table 2.
QTc =
time interval f rom D to K
√
previous RR interval
(1)
As a result, in the current version of our diagnosis
algorithm, according to the results of checking these
previous five conditions, the sensor node reports to
the base station that the heart of the monitored patient
can be suffering one of the pathologies of Table 3.
4 EXPERIMENTAL RESULTS
The complete proposed ECG-based diagnosis algo-
rithm has been ported and optimized to be executed
in the 25-channel EEG/ECG node. The statistics
and energy values shown in the rest of the paper
BIODEVICES 2009 - International Conference on Biomedical Electronics and Devices
92
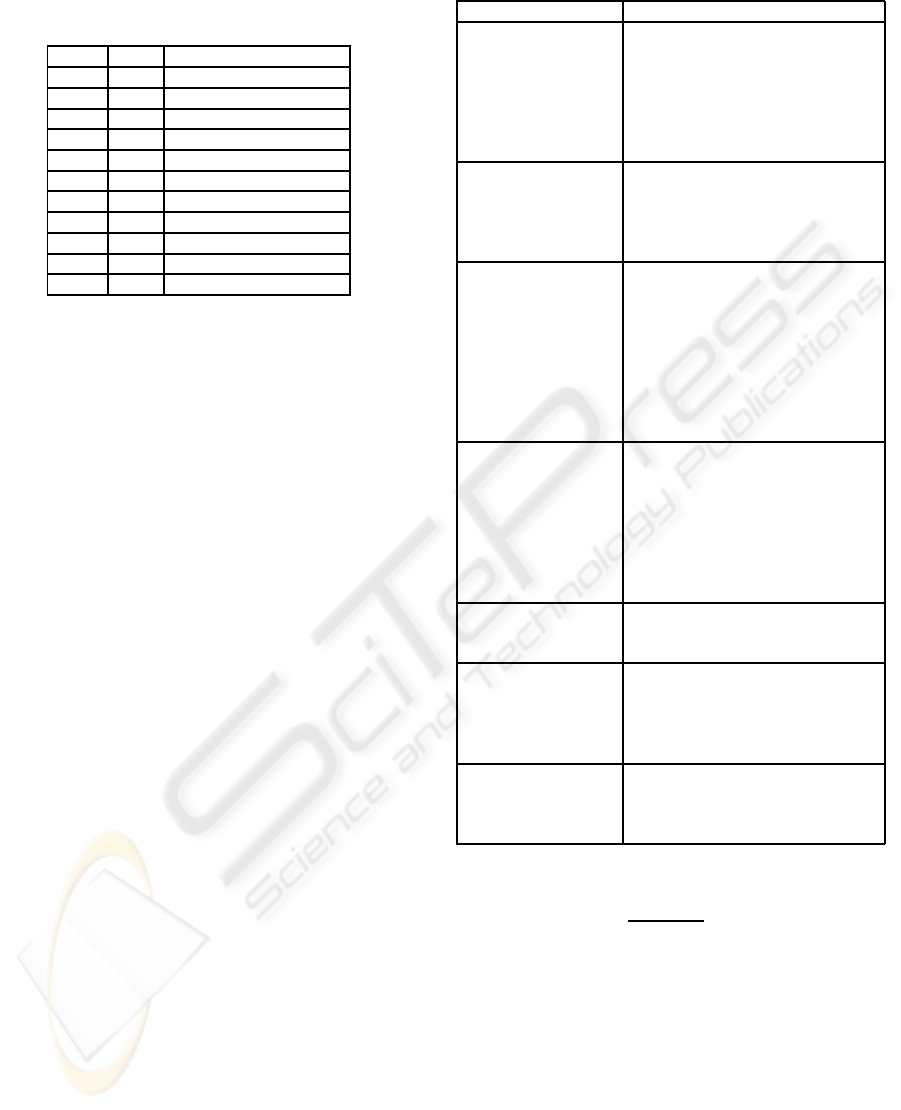
Table 2: Normal values of the QTc. HBR=Heart Beat Rate
(per minute), RR=RR interval. Values in last two columns
are in seconds.
HBR RR QTc and normal limits
40 1.5 0.46 (0.41 - 0.51)
50 1.2 0.42 (0.38 - 0.46)
60 1 0.39 (0.35 - 0.43)
70 0.86 0.37 (0.33 - 0.41)
80 0.75 0.35 (0.32 - 0.39)
90 0.67 0.33 (0.30 - 0.36)
100 0.60 0.31 (0.28 - 0.34)
120 0.50 0.29 (0.26 - 0.32)
150 0.40 0.25 (0.23 - 0.28)
180 0.33 0.23 (0.21 - 0.25)
200 0.30 0.22 (0.20 - 0.24)
were obtained using the model of the 25-channel
EEG/ECG system for PowerTOSSIM, which was val-
idated in (Rinc´on et al., 2008), showing variations of
less than 4% between the simulation framework and
the measurements of the final platform.
4.1 Validation of the ECG-based
Diagnosis Algorithm
The accuracy of the algorithm running on the 25-
channel EEG/ECG system was tested with several in-
put signals taken from the QT database (Laguna et al.,
1997). This database was specially created for eval-
uation of algorithms that detect waveform boundaries
in ECG signals. It consist of 105 fifteen-minute ex-
cerpts of two-channel ECG recordings. It also con-
tains a subset of beats (at least 30 in each recording)
that have been manually annotated by cardiovascular
analysis experts.
In our first set of experiments, we have com-
pared the performance of the proposed algorithm
with MMD and other state-of-the-art ECG detec-
tion algorithms from the literature for detection of
waveform boundaries in ECG signals: the original
MMD off-line algorithm (Sun et al., 2005), an adap-
tive thresholding-based detector (TD) (Daskalov and
Christov, 1999) and a wavelet transform-based detec-
tor (WD) (Li et al., 1995).
We report three parameters in these comparisons,
namely, their mean error (m), standard deviation (σ)
and Sensitivity (Se). We have used these parameters
because they give a complete overview of the overall
behavior of each algorithm, as m shows how close the
detection results using an algorithm are to the manu-
ally annotated results, σ represents the stability of the
detection and Se (defined in 2) measures the detection
sensitivity (where TP is the number of true detections
and FN is the number of manual annotations that are
not detected by the algorithm).
Table 3: Pathologies detected by diagnosis module.
Problem Possible pathology
Time from D to H
longer than 0.10s
(it could even reach
0.12s).
Block of the His bundle.
Supraventricular rhythm with
aberrant conduction.
Abnormal conduction over acce-
sory pathways.
Ventricular rhythm or pacemaker
rhythm.
The time interval
from A to D is
longer than 0.20s
(long PR interval).
Disorder in the conduction be-
tween atriums and ventricles at
the atrioventricular node level,
His bundle (or its branches) or
Purkinje system.
The time interval
from A to D is
shorter than 0.12s
(short PR interval).
Presence of an anomalous ac-
cesory pathway that produces a
faster conduction or the presence
of a rhythm with origin in the
atrioventricular union, in the left
atrium or in the lower part of
the right atrium. Generally, this
anomaly is due to a ventricular
preexcitation.
The amplitude of J
is negative (T wave
is negative).
Primary alterations of the repo-
larization phase (due to ischemia
or myocardial infarction, suba-
cute pericarditis or myocarditis).
Secondary alterations of the re-
polarization phase (due to alter-
ations of the ventricular repolar-
ization).
The time from D
to F is longer than
0.03s.
Delay in the ventricular activa-
tion time.
QT interval longer
than the values
specified in Table
2.
The ventricular repolarization
has slowed down, which can
be due to acquired or congen-
ital causes. It is related to the
appearance of arrhythmias.
QT interval shorter
than the values
specified in Table
2.
This problem is usually related to
the use of some medicines, hy-
percalcemia or hyperpotassemia.
Se =
TP
TP+ FN
×100 (2)
Table 4 shows the results obtained from these
comparisons and the accepted standard deviation tol-
erances given by the Common Standards for Electro-
cardiography (CSE) committee. As this table illus-
trates, the values of the mean error are quite low and
can be compared to the values obtained with MMD,
TD and WD. Only in the case of T
on
, the mean er-
ror is very high, but this is not a problem, since T
on
is not relevant for the cardiovascular pathologies tar-
getted by the diagnosis module. Then, the compari-
son between the proposed run-time ECG signal recon-
struction algorithm and the MMD detector in terms of
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS ALGORITHM FOR A WIRELESS BODY
SENSOR PLATAFORM
93

Table 4: Comparative results of our run-time ECG charac-
teristic wave detection and other state-of-the-art ECG de-
tection algorithms.
Technique Parameter P
on
P
of f
QRS
on
QRS
of f
T
on
T
of f
Ours Se(%) 92.4 92.4 100 100 96.6 91.7
m(ms) 1.4 14.9 -7.8 8.2 53.6 12.8
σ(ms) 15.6 13.3 22.6 16.8 21.6 20.9
MMD Se(%) 97.2 94.8 100 100 99.8 99.6
m(ms) 9.0 12.8 3.5 2.4 7.9 8.3
σ(ms) 9.4 13.2 6.1 10.3 15.8 12.4
TD Se(%) 96.2 97.0 99.9 99.9 98.8 98.9
m(ms) 10.3 -5.7 -7.3 -3.6 23.3 18.7
σ(ms) 14.1 13.6 10.9 10.7 28.3 29.8
WD Se(%) 89.9 89.9 100 100 99.1 99.2
m(ms) 13.0 5.4 4.5 0.8 -4.8 -8.9
σ(ms) 12.7 11.9 7.7 8.7 13.5 18.8
CSE σ(ms) 10.2 12.7 6.5 11.6 - 30.6
σ is very important, since the proposed algorithm is
based on the original off-line MMD detector. As ex-
pected, the values of the standard deviation achieved
by the MMD method with the complete signal anal-
ysis instead of the limited run-time history are better.
Nonetheless, the degradation of standard deviation in
the case of the new run-time approach is very limited.
In particular, the reasons for this limited degradation
are the following:
• The proposed run-time algorithm is optimized to
work in real-time in a sensor node platform with a
simple microcontroller. Floating point operations
are very costly in terms of time for such a sim-
ple microcontroller, and they had to be converted
into integer operations, with the resultant loss of
precision in the filtering and the multiscale mor-
phological transform operations.
• Dynamic thresholding based on the histogram of
the signal in the new approach is more difficult
than with the off-line approach, since only a small
window of data (the last 1.5s of signal) is available
to choose the correct thresholds. Sometimes this
is also a source of errors in the detections.
However, it is very important the fact that results
using the proposed run-time approach are not far from
the original algorithm, especially considering that, in
exchange of a bit of accuracy, it is possible to process
the input data in real-time and the patient can be in-
formed of a possible cardiac pathology in real-time.
Therefore, the time to react and attend the patient in
case a problem occurs is minimal, and then the conse-
quences of the problem and the probability of the ap-
pearance of a more serious pathology derivated from a
late identification of the problem are greatly reduced.
4.2 Energy Features of Diagnosis
Sensor Node Platform in WBSN
One of the main problems in WBSNs is energy con-
sumption, mainly due to the high sampling frequency
required by these applications. Sensors generate lots
Table 5: Typical ranges of heart beat rate per minute at rest
and practising aerobic and anaerobic exercise for different
kind of adult people.
Sedentary Fit Sportperson
At rest 70 - 90 60 - 80 40 - 60
Aerobic 110 - 130 120 - 140 140 - 160
Anaerobic 130 - 150 140 - 160 160 - 200
Table 6: Energy savings in the radio due to transmission
using the run-time ECG detector instead of data streaming.
Sedentary Fit Sportperson
At rest 91 - 93% 92 - 94% 94 - 96%
Aerobic 87 - 89% 86 - 88% 84 - 86%
Anaerobic 85 - 87% 84 - 86% 80 - 84%
of data that need to be transmitted to the base station,
for that reason, the time that sensors can be in stand-
by mode is shorter than in other kind of applications.
In these networks, the nodes are attached to the body,
therefore batteries must be very small, to allow the
person to do a normal life. These small batteries have
a short lifetime and after some time they need to be
replaced. If the sensors are implanted in the body, the
replacement of the batteries is not feasible. A possible
alternativecould be energyscavengers, but in general,
energy scavengers are not able to supply the node con-
tinuously, since the average power generated by one
of these devices is usually much lower than the av-
erage power consumed by the nodes. Normally, they
are coupled to batteries and recharge them, extending
their lifetime.
Analyzing the energy consumption of the different
hardware blocks of a node using typical applications
for WBSNs, we can extract that the main cause of en-
ergy waste is the transmission and reception of data
via radio. The radio is responsible for between 70%
and 90% of the total amount of energy consumed by
the whole sensor node. Then, one of the main chal-
lenges in WBSNs is trying to reduce as much as possi-
ble the energy consumption of the node, therefore we
need to minimize the energy consumed by the radio,
since the radio is the main source of energy waste.
In this section, we consider and analyze three dif-
ferent approaches: data streaming, the use of the pro-
posed run-time ECG signal reconstruction algorithm
and the complete embedded diagnosis system, cou-
pling the diagnosis module introduced in 3.2 to the
basic run-time ECG algorithm.
First, we analyze the most basic application, that
simply performs data streaming, which means that all
the data read by the sensors is transmitted to the base
station without any intermediatte operation. All the
information will be processed off-line in the base sta-
tion. In order to perform a reliable ECG streaming, a
sampling frequency of about 200Hz is required. Tak-
BIODEVICES 2009 - International Conference on Biomedical Electronics and Devices
94

ing into account that the packet payload is 18 bytes
and the size of each sample is 12 bits, we can con-
clude that 1000 packets are sent in 60s.
Using the run-time ECG signal reconstruction al-
gorithm previously described, the sampled data are
preprocessed before being sent. In this way, a packet
is sent only when a R peak is detected. The sent
packet contains when the R peak has been detected,
the position of the rest of detected points respect the
R peak and the amplitude of P peak, R peak and T
peak. The number of packets sent in 60s using this
algorithm would be equal to the heart beat rate per
minute. Typical values of heart beat rate per minute
are shown in Table 5. Table 6 shows the energy sav-
ings in the radio due to transmission of packets ob-
tained with the use of the proposed algorithm. In
order to verify these theoretical results, some exper-
iments were run in the simulator. The result of one
of these simulations is presented in Figure 3. This
plot shows that the energy consumption due to packet
transmission in the case of the ECG streaming appli-
cation is 50.30mJ in a simulation of 60 real seconds.
If the run-time ECG algorithm is used, the energy
consumption drops to 3.73mJ for an input signal of
76 heart beats per minute, which means a reduction
of 92.6%, as it was predicted in Table 6.
As previously mentioned, a diagnosis module has
been implemented and successfully tested. This mod-
ule evaluates, taking as input the points detected by
the run-time ECG signal reconstruction algorithm, if
the ECG signal of the patient is normal or it presents
any anomalous behavior. When a problem is de-
tected, a packet is sent, containint the code of the di-
agnosed pathology and the points of the wave where
the pathology was detected. In the worst case, when
a problem is detected in every heart beat, the energy
savings with regard to the data streaming case are the
same as if we do not use the diagnosis module. In the
best case, when no pathology is detected because the
ECG signal is normal, no transmission is produced
and therefore the reduction in the number of trans-
missions reaches 100% improvement.
5 CONCLUSIONS
Energy consumption minimization is one of the ma-
jor design challenges to enable WBSN-based solu-
tions for personal healthcare systems. In this paper,
we have demonstrated the feasibility of exploiting
the limited processing and storage resources to de-
ploy a novel real-time automated ECG analysis and
arrhythmia diagnosis algorithm on an actual sensor
node platform. This goal was achieved through judi-
0,00
10,00
20,00
30,00
40,00
50,00
60,00
ECG streaming Run-time ECG detector
E (mJ)
Figure 3: Energy consumption due to packet transmission
for the ECG streaming application and the run-time ECG
signal reconstruction algorithm during a period of 60s.
cious application-level optimizations, taking into ac-
count the underlying hardware architecture and the
real-time constraints of the automated diagnosis ap-
plication. The satisfactory accuracy of both the auto-
mated ECG analysis (ECG characteristics wave de-
tection) and ECG-based arrhythmia diagnosis algo-
rithms was assessed. Finally, we also demonstrated
that the deployment of these advanced algorithms for
ECG analysis and autodiagnosis enables a dramatic
reduction of the energy consumption (between 80%
and 100%, depending on the sensed signal), com-
pared to the conventional WBSN approach that sim-
ply wirelessly streams the sensed data to the central
node. These excellent results show the potential of
embedding advanced processing and intelligence in
sensor nodes for extending the lifetime of WBSNs,
and motivates further research in characterizing the
optimal trade-off between embedded signal process-
ing and wireless communications for these energy-
constrained wireless networks.
REFERENCES
Culler, D. (2006). Tinyos: Operating system design for
wireless sensor networks. Sensors, pages 41–49.
Culler, D., Estin, D., and Srivastava, M. (2004). Overview
of sensor networks. Computer, pages 41–49.
Daskalov, I. K. and Christov, I. I. (1999). Automatic detec-
tion of the electrocardiogram T-wave end. Med Biol
Eng Comput, 37(3):348–353.
Gay, D., Levis, P., von Behren, R., Welsh, M., Brewer,
E., and Culler, D. (2003). The nesC language: A
holistic approach to networked embedded systems. In
PLDI’03:Programming Language Design and Imple-
mentation.
Jovanov, E. and et al. (2005). A WBAN system for ambula-
tory monitoring of physical activity and health status:
applications and challenges. In International Confer-
ence of the IEEE Engineering in Medicine and Biol-
ogy Society.
Kemere, C. and et al. (2004). Model-based decoding for
reaching movement for prosthetic systems. In In-
IMPLEMENTATION OF AN AUTOMATED ECG-BASED DIAGNOSIS ALGORITHM FOR A WIRELESS BODY
SENSOR PLATAFORM
95

ternational Conference of the IEEE Engineering in
Medicine and Biology Society.
Khadtare, M. S. and Sahambi, J. (2004). ECG arrhythmia
analysis by multicategory support vector machine. In
AACC, pages 100–107.
Laguna, P., Mark, R. G., Goldberger, A. L., and Moody,
G. B. (1997). A database for evaluation of algorithms
for measurement of QT and other waveform intervals
in the ECG. Computers in Cardiology, pages 673–
676.
Lazzer, S., Feng, J., Koushanfar, F., and Potkonjak, M.
(2002). System-architectures for sensor networks is-
sues. In IEEE International Conference on Computer
Design (ICCD).
Li, C., Zheng, C., and Tai, C. F. (1995). Detection of ECG
characteristic points using wavelet transforms. IEEE
Transactions on Biomedical Engineering, 42:21–29.
LifeShirt. http://www.vivometrics.com.
Lo, B. and Yang, G. (2005). Key technical challenges and
current implementations of body sensor networks. In
Second International Workshop on Wearable and Im-
plantable Body Sensor Networks.
L¨ofgren, N. and et al. (2007). EEG entropy estimation using
a Markov model of the EEG for sleep stage separation
in human neonates. In International Conference of the
IEEE Engineering in Medicine and Biology Society.
Lutz Bierl, T. I. (2000). MSP430 family mixed-signal mi-
crocontroller application reports. Technical Report TI-
06-2000.
Penders, J., Gyselinckx, B., de Vicq, N., and Torfs, T.
(2007). Body area networks for multi-modal biomed-
ical monitoring. In pHealth.
P´erez-G´omez, F. (1985). Cardiac Pacing. Editorial Grouz.
Project, C. B. http://www.eecs.harvard.edu/ mdw/proj/ code-
blue/.
Rinc´on, F., Paselli, M., Recas, J., Zhao, Q., S´anchez-
´
Elez,
M., Atienza, D., Penders, J., and Micheli, G. D.
(2008). OS-Based Sensor Node Platform and En-
ergy Estimation Model for Health-Care Wireless Sen-
sor Networks. In Design, Automation and Test in Eu-
rope (DATE ’08), number ISSN: 1530-1591/05.
Schamroth, L. (1971). The disorders od cardiac rhythm.
Blackwell Scientific Publications.
Semiconductor, N. (2000). nRF2401 transceiver data
sheets. http://www.nordicsemi.com/.
SmartShirt. http://www.sensatex.com.
S¨ornmo, L. and Laguna, P.(2005). Bioelectrical Signal Pro-
cessing in Cardiac and Neurological Applications. El-
sevier Academic Press.
Sun, Y., Chan, K. L., and Krishnan, S. M. (2002). Ecgsignal
conditioning by morphological filtering. Computers in
Biology and Medicine, 32(6):465–479.
Sun, Y., Chan, K. L., and Krishnan, S. M. (2005). Charac-
teristic wave detection in ecg signal using morpholog-
ical transform. BMC Cardiovascular Disorders.
BIODEVICES 2009 - International Conference on Biomedical Electronics and Devices
96
