
A MODEL TO OPTIMIZE THE USE OF IMAGING EQUIPMENT
AND HUMAN SKILLS SCATTERED IN VERY LARGE
GEOGRAPHICAL AREAS
Daniel Ferreira Polónia, Carlos M. A. Costa and José Luís Oliveira
DETI/IEETA, Universidade de Aveiro
Campus Universitário de Santiago, 3810-193 Aveiro, Portugal
Keywords: Health Information Systems, Radiology Information Systems, Teleradiology, Ubiquitous Systems, CSCW.
Abstract: Recent studies have shown that the good geographical coverage of Imagiologic Information Systems and
equipment such as Picture Archiving and Communication Systems (PACS) is not matched by similar
coverage levels of radiologists, especially in rural and academic health institutions. In this paper, we address
this problem proposing a solution that is twofold, with the first one being process based, through the
optimization of work assignment within pools of human resources according to Service Providers
availability, and the second part being technology based, through the interconnection of all the health
institutions PACS equipment and radiologists geographically dispersed. After describing the high level
solution, we present some of the results of the implementation of this concept and some of the technical
challenges still to overcome. Finally, the conclusion chapter presents the impact of the system in the
involved institutions.
1 INTRODUCTION
During the last 10 years, the use of digital medical
imaging systems increased tremendously inside
healthcare institutions (Reiner, Siegel et al. 2003),
representing today one the most valuable tools
supporting the medical decision process and
treatment procedures.
Initially, the benefits of digital technology were
confined to the equipment machines and to the
relatively few examples of image data migration into
a centralized shared archive, for posterior utilization.
The medical imaging digitalization and the
implementation of PACS, Picture Archiving and
Communication Systems, enabled practitioner’s
satisfaction through improved, faster and ubiquitous
access to image data (Costa, Oliveira et al. 2005).
Moreover, it reduced the costs associated to the
storage and management of image data and it
increased the intra and inter-institutional data
portability (Costa, Silva et al. 2004). In fact, one the
most important benefits of digital medical imaging is
to allow widespread sharing and remote access to
medical data outside institutions. This type of
system presents an opportunity to improve
cooperative work among groups, taking place within
or across healthcare institutions. With PACS a new
saying emerged: “Any Image, Anywhere and at Any
Time”.
2 MATERIALS AND METHODS
The most important contribute to the exchange of
structured medical image was the establishment of
DICOM, Digital Imaging and Communications in
Medicine, standard in 1992. Medical images in
electronic format opened doors to numerous post-
processing techniques that allow extraction of more
and better information from the acquired data.
However, modelling and quantitative imaging
analysis tools are especially expensive regarding
software packages and computational power
requirements, thus becoming a very scarce goods,
that, although are available 24 hours a day, are only
used for a few hours (Reiner, Salkever et al. 2005).
Most statistical data and productivity studies
show us that medical image data can be generated in
practically any healthcare institution, even with
limited human or financial resources (Reiner, Siegel
et al. 2002). However, the expensive computational
tools and the human skills are usually concentrated
in a reduced number of specialized medical centres,
and there is no direct relationship between the
208
Ferreira Polónia D., M. A. Costa C. and Luís Oliveira J. (2007).
A MODEL TO OPTIMIZE THE USE OF IMAGING EQUIPMENT AND HUMAN SKILLS SCATTERED IN VERY LARGE GEOGRAPHICAL AREAS.
In Proceedings of the Ninth International Conference on Enter prise Information Systems - SAIC, pages 208-212
DOI: 10.5220/0002394902080212
Copyright
c
SciTePress

existence of digital imaging equipment and the
existence of sophisticated software and highly
skilled technicians and examiners (Reiner, Siegel et
al. 2005).
Our research question was centred in the
following motto: Is there a way to optimize the even
distribution of equipment across the country and the
uneven distribution of software analysis packages
and skilled examiners using technology and
processes for trans-institutional use of resources
from the equipment and human point of view?
2.1 “As is” Scenario
As shown previously, most studies show us that
there is a good distribution of hospitals and
radiological equipment across the country in which
it is not matched by the distribution of resources
(physicians and radiologists) nor by the productivity
of the equipment (number of exams made by that
equipment).
In the Portuguese case, the National Health
Service shows, in its statistical data (Saúde 2004),
that most of its secondary care institutions possess
PACS equipment and a radiology technician.
However, if we measure the productivity ratio of
each of this equipment we reach the conclusion that
most of the equipment is under utilized, either by
lack of appropriate human and technical resources to
perform a quick follow up on the patient situation,
and either by lack of external clients that acquire
services to the institution, thus maximizing
equipment productivity.
Most of the institutions are properly equipped
with PACS software acquisition modules, including
digital image modalities interfaces, also known as
“dicomizers”, that run over appropriate internal
institutional LAN infrastructures and that are
connected among themselves through a private
governmental network infrastructure, the RIS,
acronym for Rede de Informação da Saúde, (Saúde
2006) that interconnects to the Internet. Also, staff
that operates this equipment is considerably skilled
in managing and operating its basic features, through
multiple periodic training actions made by
equipment vendors.
However, these institutions have difficulties in
recruiting and/or economically supporting specialists
(full time or partially) like, for instance, a physician
radiologist. So, these hospitals engage external
services to third party service providers, in the form
of institutions or singular persons, to perform
detailed examinations and provide feedback to the
institution physician.
These entities have remote access to the
institution PACS and the communication is
established in a “peer-to-peer” architecture,
supported by a VPN channel that connects to the
institution LAN.
The system requires a high speed internet
connection (or private dialup link) and a specific
client PACS application installed on remote PCs.
Many times, these external specialists are physically
distant more than 300 kilometres away.
2.2 Proposed “to be” Model
First of all, the proposed model assumed that all
equipment that joins the system uses the technical
norm DICOM v3 as support format for archiving
and transmitting medical imaging among the
different partners (DICOM).
In our model, we have a twofold approach to
optimize the use of computational resources and
human skills scattered in very large geographical
areas. The first is a process-based approach where,
from analysing the human resources and software
infra-structure available, a process optimization
method is developed. The second approach is a
technical one where the required technological
infrastructure is described, demonstrating the
information workflow and the way it is possible to
optimize the existing systems.
2.2.1 Process Based Approach
From the process side (including economic, human
and computational perspectives), first of all, it is be
necessary to make an inventory of all the interested
parties in participating in the process, either as
Client Institution (the one that performs the
Service Requests and feeds the system with data to
be serviced), either as Service Provider (the one
that gathers the data to be serviced, downloads it,
performs the requested service and uploads it again
to the Client Institution).
The Client Institution is identified according to
the type of institution ,i.e., clinical practice, hospital,
etc.; the Users allowed to access, the type of
Modalities that are attached to the PACS system
and a Track Record of the requested services,
including the number of providers requested for each
service and their experience level. Each Client
Institution has the ability to, optionally and
according to the status of the user which performs
the request, includes the specific type of expertise
required by the provider and if any specific type of
equipment is necessary, thus maximizing the
existing equipment and computational power
available by the pool of Service Providers. Also as
A MODEL TO OPTIMIZE THE USE OF IMAGING EQUIPMENT AND HUMAN SKILLS SCATTERED IN VERY
LARGE GEOGRAPHICAL AREAS
209
an option, a priority level for the Service Request
can be attached, thus defining minimum and
maximum response time.
According to the complexity level required for
each Service Request, a given number of tokens is
automatically assigned by the Client Institution
Interface Engine (Figure 1), based on the number
of examiners, experience level, expertise required,
equipment required and priority level. These tokens
determine the “virtual value” to be paid by the Client
Institution to the Service Provider for the service
requested (Prinz 1999).
The Service Provider is identified according to
the type of institution that it belongs to (free lancer,
clinical practice, hospital, etc.), the experience level
that possesses, the type of expertise that it has and
the equipment available. It also has attached
information concerning service level agreements
such as minimum and maximum response time to a
request that it must contractually meet.
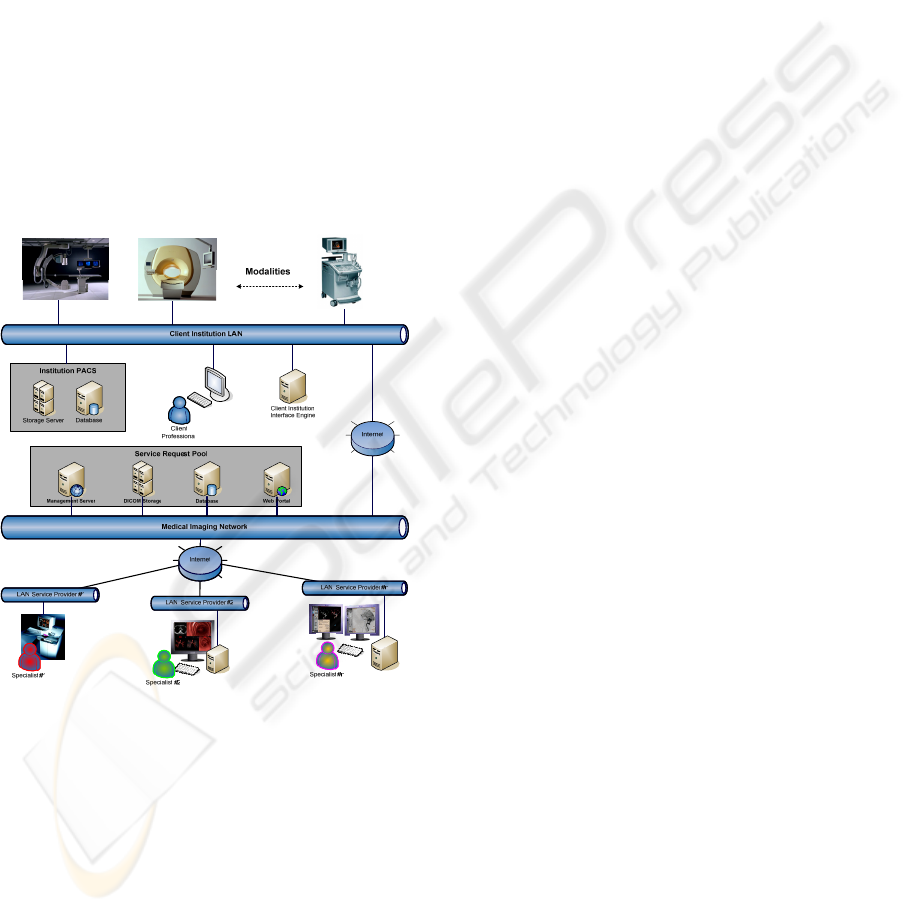
Figure 1: PACS based Service Request Pool.
Providing a use case, we have the following:
Once the exam is performed in an Image
Modality of the Client Institution (Figure 1), it is
placed in the Institution PACS and the Client
Professional, examines it, determining that it needs
a service to be provided by a number of specialists
in the field, with a certain priority level and,
eventually, requiring the use of specific equipment.
The Service Request is then placed in Client
Institution Interface Engine where its clinical
information is anonymized. It is also attached some
information concerning clinical data, inserted as a
DICOM structured report file (Noumeir 2003).
The Service Request is then sent through the
Internet (or a Virtual Private Network) to a Medical
Imaging Network that has attached to it a Service
Request Pool, where the exam is placed.
The Service Request Pool Web Portal (Figure
1) shows a personalized view to each Service
Provider, where the Service Request that is most
likely to fit its profile comes on top, followed by a
series of all the other it can execute according to its
profile.
Once a Service Provider selects a Service
Request, it counts down the number of reviewers for
that Service Request. If the number reaches zero, it
will disappear from the “pending” list in the web
portal. A Service Provider can only select
simultaneously up to a predetermined number of
service requests, thus preventing a Service Provider
from gathering the most interesting (or profitable)
Service Requests.
Another feature included is to increase the
number of tokens associated with a Service Request
at a given rate as time passes by, thus guaranteeing
that, at a given point, all exams are sufficiently
attractive to receive a response from the Service
Provider.
After performing the service requested, and
according to a Service Level Agreement to be
negotiated the moment the Service Provider joins the
system, based on the number of tokens associated
and the time that it took to perform the service, a
number of credits will be assigned to its “virtual
purse”, coming out from the Client Institution
“virtual purse”.
Once the service is concluded, data not only is
returned to the Client Institution Interface Engine
to be “de-anonymized” and sent the requiring
clinician, but it can also be kept, under its
anonymized form, in the Service Request Pool
Database so that an optional random Quality
Control review (Treitl, Wirth et al. 2005) can be
made a posteriori by a panel of reviewers that can,
based on these controls, change the Service Provider
experience level and/or type of expertise.
The same system that filters the data in the
Service Request Pool for Quality Control can also
have other utilizations like, for instance, keep data to
be used in epidemiological and scientific studies
(Krug, Bottge et al. 2003) where researchers can
gather anonymised data to be inserted into clinical
and/or research studies and where Service Providers
can reference previous cases to fundament their
decisions.
ICEIS 2007 - International Conference on Enterprise Information Systems
210
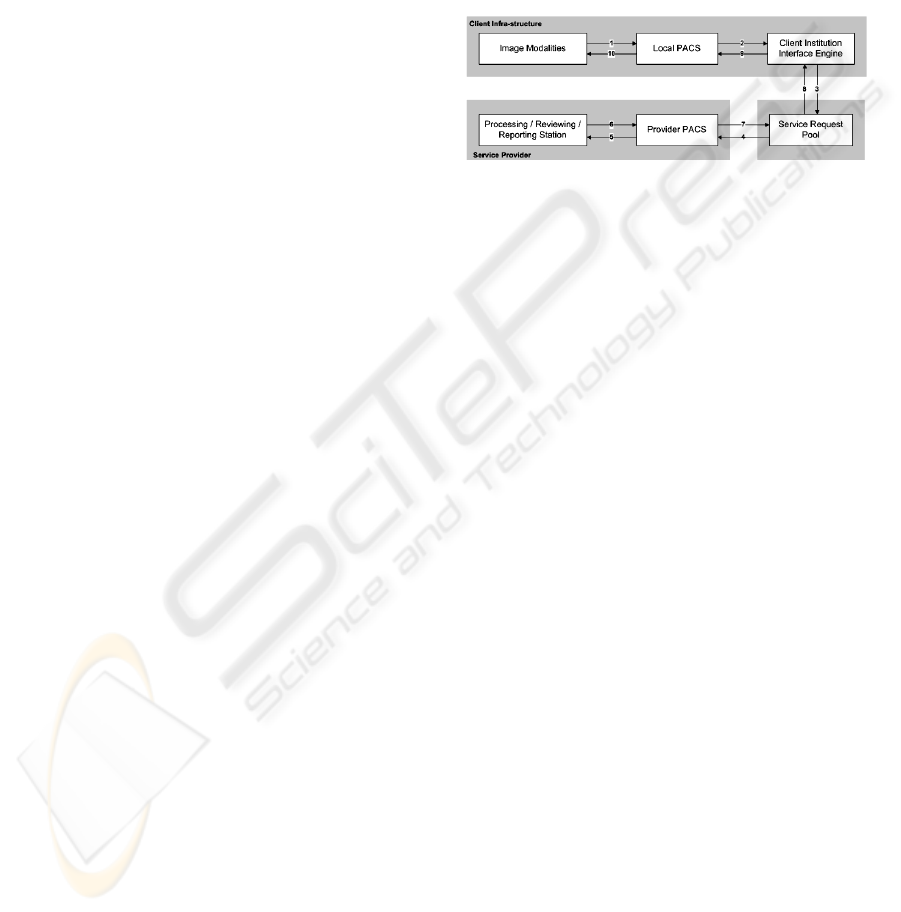
2.2.2 Technology based Approach
The technological approach, consists in
implementing an information gatherer in every
institution that adheres to the system, which
interconnects the institution PACS, that by itself
interconnects the existing modalities, (Figure 2 –
step 1). Thus it is able, through the Client Institution
Interface Engine, to receive the data from the
institution PACS in DICOM format, anonymize the
patient identification data in the DICOM headers,
label them with an internal ID number, ID request,
as well as service priority and service code intended
from the structure.
It should be noticed that the ability of radiology
technicians to operate modality equipment, to use
the PACS system and to perform basic imaging
adjustment such as brightness or contrast adjustment
is not jeopardized by the introduction of this engine.
Since PACS systems have the ability to
configure external DICOM servers to export
imaging procedures, in this case it is added a new
export unit to the local PACS system designated
“PACS POOL”. In order to use this functionality,
the radiology technician only has to select the
intended information and “Send to PACS POOL”
(Figure 2 – step 2), just like when a DICOM image
is sent to another server or institution nowadays.
Whenever it is necessary to add extra clinical
data to support the intended service code (patient
history, lab analysis, etc.), this information can be
given as a DICOM file of the type Structured
Report. In this DICOM file it can also be included
the specification of the intended service,
represented, for instance, as an ICD10 or as
ontology. The specification can also be placed in a
“DICOM Private Tag” especially inserted.
Once the service request is inserted in the POOL
(Figure 2– step 3), i.e.: the medical images are
stored to the “DICOM Storage” and the “Database”
is updated with a new request in “pending” status,
the Service Request Pool Web Portal informs all
suitable Service Providers that there is a pending
request for that specific type of clinical service.
Once a Service Provider shows interest in analysing
that request, it passes from the state of “pending” to
the state of “lock” and it is automatically sent to the
service provider PACS system (Figure 2– step 4).
The Service Provider then processes the request
according to the request made earlier (Figure 2 –
steps 5 and 6) and sends back to the Service Request
Pool the complete process (Figure 2 – step 7). The
service results (images and reports) are, once again,
supported and transferred using DICOM standard
(Storage Syntax and Communications Protocol).
In the Service Request Pool, the Service Request
is passed from “lock” to “complete” in the “Web
Portal” and the results are sent back to the requesting
Client institution (Figure 2– step 8) i.e.: to the
Interface Engine of the Client institution.
Once arrived here, the patient identification data
is reset to all DICOM headers and the information
sent to the “Local PACS” (Figure 2– step 9) where
the results and the requested service are available for
the clinician that requested the service (Figure 2–
step 10).
3 RESULTS
With the conceptual model previously proposed, we
point to a solution to several problems that now
impairs the optimal provision of radiological
services, such as the imbalance in the distribution of
equipment and specialists over wide geographical
areas, reducing the response time and establishing a
virtual market for the provision of radiological
services.
This virtual market has a set of features such as
the ability to set up an Engine that acts as a broker
that guarantees functionalities such as:
• Double blind review of the exam if desired (the
Client Institution may not know the identity of
the Service Provider and the Service Provider
may not know the identity of the Client
Institution and the Patient that it is reviewing,
with the broker being able to reverse this
situation at any time),
• Quality of service in terms of time and
expertise (every request gets serviced through
an embedded priority management system),
• Review of the quality of service provided
(every service request processed can, randomly,
go to a database where an expert committee
samples them in order to grade the Service
Providers),
• Build up of an anonymized studies database for
epidemiological and scientific reference
analysis and fundament decisions,
• Set up a virtual market where only the most
appropriate service request are presented to the
Service Providers, performing a previous
Figure 2: A PACS based management of resources.
A MODEL TO OPTIMIZE THE USE OF IMAGING EQUIPMENT AND HUMAN SKILLS SCATTERED IN VERY
LARGE GEOGRAPHICAL AREAS
211

filtering of all the requests not suitable, and
listing them according a list of preferences set
by the Service Provider, and
• Perform administrative and financial
management of the system, guaranteeing
payment of the Service Providers by the Clients
through a token-based system that prices the
service according to its complexity, response
time and expertise of the service provider
required.
4 DISCUSSION
The implementation of such a network will be of
utmost interest for well implemented nationwide
networks of PACS infra-structures, usually owned
by National Health Service and/or by large insurance
companies in order to optimize turn-around times of
detailed diagnosis by external specialists and will
also be of interest for insurance companies that have
insurance policies options that enable the extension
of the quality of service provided to the speed of
response time, quality of the service provider and/or
the number of service provisioners.
The use of ontologies in the processing the
request in (Figure 2 – steps 5 and 6) will enable the
possibility of extending the network at a pan
European and/or at a worldwide level (admitting that
there are no ethical and legal problems with the
mutual recognition of service providers), in
extraordinary cases such as rare malformations or in
cases that require a specific expertise and/or
software only available outside the network.
From the purely economical point of view, and
abstracting the legal and ethical problems associated,
a global market could be established, thus
transforming a purely local market onto global
network of service providers, thus making available
a set of expertise and software anywhere and at any
time.
5 CONCLUSION
This entire model is designed so that there is no need
in changing the existing institutional PACS structure
of the entities involved, with no need for additional
hardware or applicational software and with a quick
learning curve for the clinical staff involved.
Furthermore, the underlying economic rationale
allows an optimization in the use of resources,
creating mutual benefits for the parties involved in
the service provisioning.
ACKNOWLEDGEMENTS
The present work has been funded by the European
Commission (FP6, IST thematic area) through the
INFOBIOMED NoE (IST-507585).
REFERENCES
Costa, C., J. L. Oliveira, et al. (2005). "Data management
and visualization issues in a fully digital
echocardiography laboratory." Biological And
Medical Data Analysis, Proceedings 3745: 13-21.
Costa, C. M. A., A. Silva, et al. (2004). "Himage PACS: A
new approach to storage, integration and distribution
of cardiologic images." Medical Imaging 2004: Pacs
And Imaging Informatics 5(25): 277-287.
DICOM Digital Imaging and Communications in
Medicine version 3.0, ACR (the American College of
Radiology) and NEMA (the National Electrical
Manufacturers Association).
Krug, B., M. Bottge, et al. (2003). "Quality control of
outpatient imaging examinations in North Rhine-
Westphalia, part I." Rofo-Fortschritte Auf Dem Gebiet
Der Rontgenstrahlen Und Der Bildgebenden
Verfahren 175(1): 46-57.
Noumeir, R. (2003). "DICOM structured report document
type definition." Information Technology in
Biomedicine, IEEE Transactions on 7(4): 318-328.
Prinz, A. (1999). "Money in the real and the virtual world:
money, money and the demand for money."
NETNOMICS 1(1): 11-35.
Reiner, B., E. Siegel, et al. (2002). "SCAR Radiologic
Technologist Survey: Analysis of Technologist
Workforce and Staffing." Journal of Digital Imaging
15(3): 121-131.
Reiner, B., E. Siegel, et al. (2003). "Evolution of the
Digital Revolution: A Radiologist Perspective."
Journal of Digital Imaging 16(4): 324-330.
Reiner, B. I., D. Salkever, et al. (2005). "Multi-
institutional Analysis of Computed and Direct
Radiography: Part II. Economic Analysis." Radiology
236(2): 420-426.
Reiner, B. I., E. L. Siegel, et al. (2005). "Multi-
institutional Analysis of Computed and Direct
Radiography: Part I. Technologist Productivity
10.1148/radiol.2362040671." Radiology 236(2): 413-
419.
Saúde, IGIF Ministério da. (2004). Primary and Secondary
Care Statistics. Lisbon, Instituto de Gestão Informática
e Financeira do Ministério da Saúde.
Saúde, IGIF Ministério da (2006). Rede Informática da
Saúde. Lisbon, Instituto de Gestão Informática e
Financeira do Ministério da Saúde.
Treitl, M., S. Wirth, et al. (2005). "Possibilities for
workflow optimization in radiology departments
beyond RIS and PACS Maglichkeiten der
Optimierung des Workflows in radiologischen
Abteilungen jenseits von RIS und PACS." Der
Radiologe 45(8): 712-723.
ICEIS 2007 - International Conference on Enterprise Information Systems
212
