
DIAGNOSIS OF DEMENTIA AND ITS PATHOLOGIES USING
BAYESIAN BELIEF NETWORKS
Julie Cowie, Lloyd Oteniya
Dept. of Computing & Mathematics, University of Stirling, Stirling, FK9 4LA, UK.
Richard Coles
Kildean Hospital, Stirling, FK8 1RW, UK.
Keywords: Bayesian Belief Networks, Dementia Diagnosis.
Abstract: The use of artificial intelligence techniques in medical decision support systems is becoming more
commonplace. By incorporating a method to represent expert knowledge, such systems can aid the user in
aspects such as disease diagnosis and treatment planning. This paper reports on the first part of a project
addressing the diagnosis of individuals with dementia. We discuss two systems: DemNet and PathNet;
developed to aid accurate diagnosis both of the presence of dementia, and the pathology of the disease.
1 INTRODUCTION
The assessment and correct management of
individuals with dementia is complex, and requires a
high level of expertise. The first stage of our
research has focused on the development of a
disease diagnosis system. The system can be viewed
as two parts: DemNet which aids a clinical decision
maker in diagnosing the likelihood of dementia; and
PathNet which provides a dementia consultant with
an indication of the possible disease(s) causing the
dementia. Both systems utilise the technique of
Bayesian Belief Networks (BBNs) to provide
probabilistic information pertaining to the presence
of dementia and likely pathologies. The BBN
formalism offers a natural way to represent the
uncertainties involved in medicine when dealing
with diagnosis, treatment selection, planning, and
prediction of prognosis (Gill et al., 2005). This is
due to the fact that the influences and probabilistic
relations among variables can be described readily in
a BBN, alternatively thought of in terms of cause-
effect relationships. Another attractive feature of the
formalism is that any probabilistic statement (often
causal) can be computed, where the user may wish
to query either a single variable, or more commonly,
combinations of variables. Further advantages of
using BBNs over other techniques are the flexibility
of the networks in the amount of information they
receive and their transparency in detailing why a
particular decision was reached. Techniques such as
decision trees can be difficult to use when only
partial information is available and other techniques
such as Artificial Neural Networks (ANNs) fail in
providing a sufficiently good explanation facility,
making it difficult for users to determine factors that
have contributed to the decision.
In this paper, we begin by providing the reader
with a brief description of the dementia syndrome,
common pathologies, and current ways in which the
disease is diagnosed. The two prototype systems
developed, DemNet and PathNet are then discussed
in detail. The paper concludes with a report on
preliminary findings and the potential for future
work.
2 DEMENTIA
2.1 About Dementia
Dementia is a term used to describe a syndrome
caused by a variety of brain disorders that have in
common a loss of brain function, which is usually
progressive and eventually severe (Alzheimer’s
Society, 2005). Symptoms of dementia may
291
Cowie J., Oteniya L. and Coles R. (2006).
DIAGNOSIS OF DEMENTIA AND ITS PATHOLOGIES USING BAYESIAN BELIEF NETWORKS.
In Proceedings of the Eighth International Conference on Enterprise Information Systems - AIDSS, pages 291-295
DOI: 10.5220/0002441802910295
Copyright
c
SciTePress

include: loss of memory, confusion and problems
with language, executive function, and social
function. The clinical decision support system
(CDSS) we have developed focuses on providing
support in diagnosing dementia and distinguishing
between the four most common dementias of old
age: Alzheimer’s disease (AD), Vascular dementia
(VaD), Dementia with Lewy bodies (DLB), and
Fronto-temporal dementia (FTD).
The current method adopted for diagnosing
dementia involves evaluation of the clinical
syndrome based on history and examination,
supported by screening investigations, and, where
appropriate, additional more specialised
investigations. In progressive degenerative
dementias, during the very early stages cognitive
deficits are usually subtle and their manifestations,
though representing change from pre-morbid
function in an individual, may remain within the
normal range for the general population. This
presents considerable challenges to early diagnosis.
However, early diagnosis and an understanding of
the underlying pathologies is of value in planning
treatment and, in some cases, initiating specific drug
intervention.
Systems to aid in medical decision making, and
in particular, disease diagnosis were introduced in
the medical field over 25 years ago. Despite their
potential usefulness in helping to provide early and
accurate diagnosis, relatively few are in general use
(Kaplan, 2001). This can be attributed to the
difficulties of integrating such systems into a clinical
setting which can generally be described as complex
systems consisting of involved algorithms,
procedures, and protocols. By addressing this
complexity and our continued interaction with those
who would potentially use the clinical decision
support system (CDSS), we hope to ensure our
system is adopted and is found a useful aid in the
diagnosis procedure.
2.2 Disease Diagnosis Systems
Many different operational research and artificial
intelligence techniques have been adopted by
CDSSs. Such techniques include the use of
mathematical models (Werner and Fogarty, 2001),
neural networks (Dybowski et al., 1996) and more
recently, optimisation techniques (De Toro et al.,
2003). Further details of the use of such techniques
are detailed in Oteniya et al, 2005.
CDSSs have also been developed that address
the specific area of dementia diagnosis. García-
Pérez et al. (1998) use data mining and neural
network techniques and Mani et al (1997) apply
decision-trees and rule-based approaches to
differentiate between Alzheimer’s disease and
Vascular dementia.
Our CDSSs extend such systems by providing a
means of identifying the presence of dementia and
the likelihood of underlying pathologies. In addition,
by using BBNs, our systems overcome some of the
difficulties other data mining techniques can present
(as detailed in Section 1).
3 DEMNET
DemNet uses a probabilistic model of dementia
diagnosis that incorporates patient history features
and physical findings. In an attempt to optimise user
friendliness and utility in a busy primary care
setting, the model seeks to use as numerically few
and as simple to use parameters as is consistent with
reasonably high diagnostic accuracy. DemNet is
described in terms of two components: the user
interface and underlying BBN. Each node of the
BBN relates to a question asked of the user. The
more answers to questions the user can provide, the
more accurate the system in diagnosing the presence
of dementia.
DemNet is designed to be used by clinical
practice nurses, who are involved in the primary
level assessment of patients.
In order to facilitate a hand crafted BBN,
information was elicited from our domain expert (a
practicing dementia consultant) via a number or
technical workshops. The process involved deciding
on key diagnostic variables and the relationships
between them, as well as quantifying the relations
probabilistically. In an attempt to optimise user
friendliness and utility in a busy primary care
setting, the models seeks to use as numerically few
and as simple to use variables as is consistent with
reasonably high diagnostic accuracy. This process
brought to light both advantages and disadvantages
of this technique. Further information on these, the
elicitation process and the methodology adopted is
given in Oteniya et al, 2006..
3.1 The Bayesian Belief Network
The underlying DemNet BBN is given in Figure 1.
In the model, the nodes on the periphery of the
network collect evidence relating to: the individual’s
current functioning, global severity of cognitive
impairment, individual’s age, duration of
ICEIS 2006 - ARTIFICIAL INTELLIGENCE AND DECISION SUPPORT SYSTEMS
292
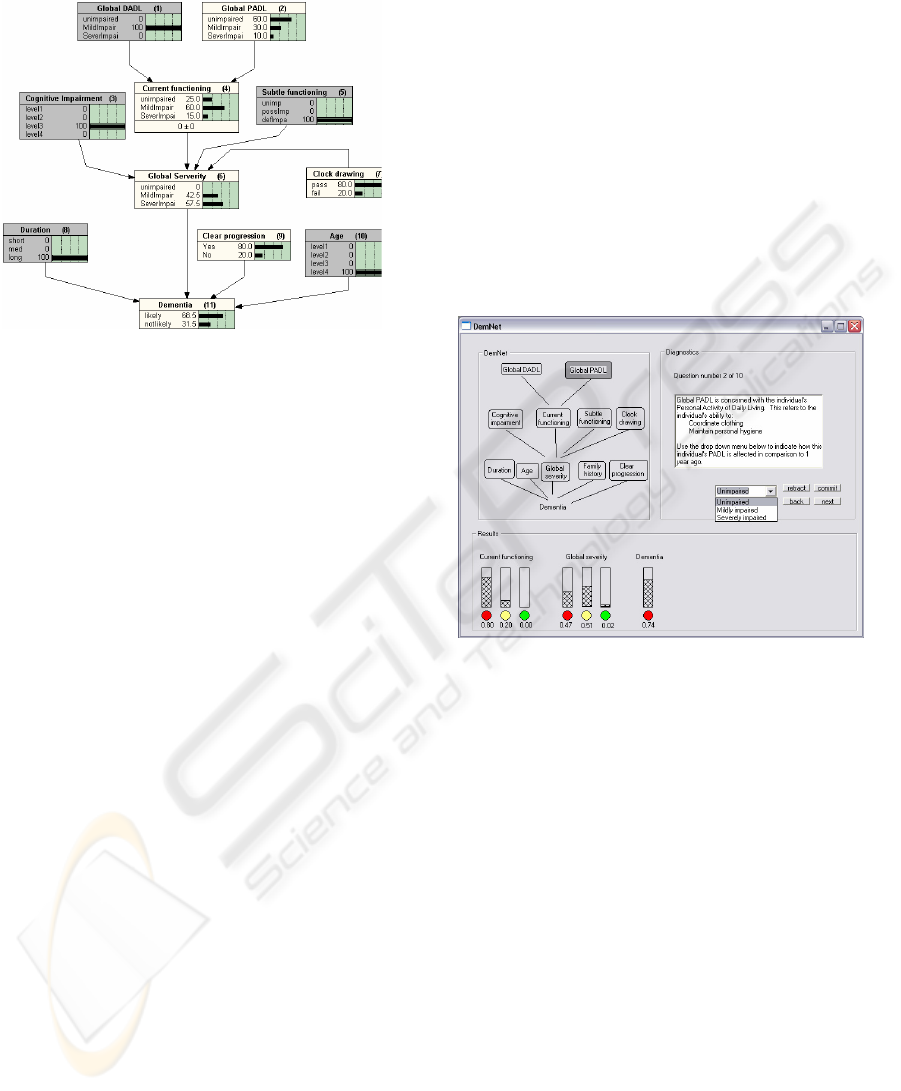
impairment, and whether clear progression is
identifiable.
Figure 1: DemNet Bayesian Belief Network.
With each piece of evidence presented, the model
recalculates the posterior probability of the related
child nodes. For example, in our model, the state of
node 4 (current functioning) combined with
evidence presented to nodes 3, 5, and 7 will cause
the recalculation of posterior probabilities for child
nodes 6 and 11. This implies that information given
regarding the level to which cognition is impaired
(node 3) and the degree to which subtle functioning
is effected (node 5), combined with the state of
current functioning (node 4), influences a patient’s
global severity (node 6) and ultimately the
likelihood of the patient having dementia (node 11).
The network also incorporates the level of influence
which data has on increasing a related node’s
probability. In Figure 1, we can see that a subset of
information has been provided about a given patient
(denoted by dark grey nodes). Given the
information provided, we can see that this patient
has a 69% chance of having dementia.
3.2 User Interface
An intuitive user interface guides the user through a
series of questions representative of each node in the
BBN. This interface is depicted in Figure 2. The
interface is divided into 3 areas, namely the model
pane, diagnostic pane, and results pane. The model
pane displays the underlying DemNet model which
can be helpful to the user in identifying which pieces
of data they have provided (denoted by dark grey
nodes) and some notion of how each piece of data
relates to the diagnosis given. The diagnostic pane
displays the question associated with a selected
diagnostic node. Each node has a number of possible
states. Each of these states relate to possible answers
to the diagnostic questions. The user is therefore
restricted in the response they give by choosing the
appropriate answer from a drop down menu. The
results pane for DemNet shows 3 sets of results
relating to current functioning, global severity, and
dementia. The first two sets of bars in the results
pane relate to nodes in the model that are crucial to
determining whether dementia is present, and are
nodes which rely heavily on the answers/evidence
given to other nodes. The three bars associated with
Current Functioning and the three bars associated
with Global Severity are representative of the 3
states possible for these nodes. The dementia bar
indicates the likelihood of the disease being present.
Figure 2: DemNet User Interface.
4 PATHNET
PathNet is an extension of DemNet for use by
domain experts (usually dementia consultants)
within the primary care setting. The system allows
the decision maker to identify the underlying
pathologies of a given case of dementia. A number
of different pathologies can lead to the syndrome of
dementia, either singly, or in combination. It is the
four most common dementias of later life:
Alzheimer’s disease, Vascular dementia, dementia
with Lewy bodies and Fronto-temporal dementia
that PathNet aims to identify.
As with DemNet, the system can be divided into
the user interface and underlying BBN. As the
dementia syndrome may be caused by multiple co-
existing pathologies, we have designed our model
such that it is capable of identifying the likelihood of
different types of dementia, either singularly, or, as
is often the case, co-existing with other dementia
DIAGNOSIS OF DEMENTIA AND ITS PATHOLOGIES USING BAYESIAN BELIEF NETWORKS
293

diseases. In addition, if dementia is suspected, but
none of the four most common pathologies can be
identified, the system indicates the presence of
dementia (other), that is, a form of dementia not
identified by the system.
Figure 3: PathNet results pane.
The PathNet interface is identical in layout to the
DemNet Interface but has one main difference in the
results pane. This incorporates information relating
to the likelihood of the different dementia
pathologies. This is shown in Figure 3. As can be
seen from Figure 3, the user is provided with a
visual representation of the probability distribution
across each of the diseases.
5 CURRENT FINDINGS AND
FUTURE WORK
5.1 Evaluation of Prototypes
To date, validation of the systems has involved a
workshop with expert physicians and informal
discussions with expert clinicians in the field. The
main purpose of the workshop was to discuss the
structure of the model, that is the variables and their
relations, and secondly, to discuss the validity of the
diagnostic output of the model for a number of
trivial and non-trivial typical scenarios. Recently,
we have initiated a small clinical trial which seeks to
collect clinical data relating to the diagnosis of
dementia and the pathologies. Once the data
collection study is complete (anticipated to be
October 2006), we will analyse the data using a tool
currently being developed which automatically
learns the structure and parameters from a given
dataset (see Section 5.2). This new model will be
compared with the hand-crafted models developed
to date.
5.2 Inducing the Network
Current work is focused on collecting data from
clinical practitioners conducting dementia diagnosis.
We hope to build up a sufficient body of data to be
able to induce a BBN, and ultimately compare the
structure and diagnostic accuracy of the network
derived with original hand-crafted models, allowing
insight into the potential advantages and
disadvantages of each approach for building BBNs.
6 CONCLUDING COMMENTS
Although this research is still in its preliminary
stages, we feel confident that the systems developed
have great potential in aiding in dementia diagnosis.
Through presentations and informal discussions, we
have been able to gain some initial feedback from
practitioners involved in this area. This feedback
has been extremely enthusiastic and encouraging.
Over the next few months we hope to be able to
produce some results from the comparison with the
data-derived BBN and the expert-derived BBN.
These results will hopefully give useful indication of
the benefits of each approach as well as provide
insight for the direction of future research. Further
details of the project can be found on the project
website: http://www.cs.stir.ac.uk/~lot/dotpi/
REFERENCES
Alzheimer’s Society. (2005). Facts about dementia,
Alzheimer’s society, Dementia care and research.
Retrieved January 20, 2006, from
http://www.alzheimers.org.uk/Facts_about_dementia/
How_dementia_progresses/index.htm
de Toro F.J., Ros, E., Ortega, J. (2003). Non-invasive
Atrial Disease Diagnosis Using Decision Rules: A
Multi-objective Optimisation Approach. In
Proceedings of 2
nd
International EMO Conference,
pages 638-647, Faro, Portugal, April 2003. Springer-
Verlag.
Dybowski, R., Weller, P., Chang, R., Gant, V. (1996).
Prediction of outcome in the critically ill using an
artificial neural network synthesised by a genetic
algorithm. The Lancet, 9009(347): 1146-1150.
García-Pérez, E., Violante A., Cervantes-Pérez, F. (1998).
Using neural networks for differential diagnosis of
Alzheimer disease and vascular dementia. Expert
Systems with Applications, 1-2(14): 219-225.
Gill, C.J., Sabin, L., Schmid, C.H. (2005). Why clinicians
are natural Bayesians. British Medical Journal 330:
1080 – 1083
Kaplan, B. (2001). Evaluating informatics applications -
clinical decision support systems literature review.
International Journal of Medical Informatics, 1(64):
15-37.
Mani, S., Shankle, W.R., Pazzani, M.J., Smyth, P. Dick,
M.B. (1997). Differential Diagnosis of Dementia: A
Knowledge Discovery and Data Mining (KDD)
ICEIS 2006 - ARTIFICIAL INTELLIGENCE AND DECISION SUPPORT SYSTEMS
294

Approach. J. of American Medical Informatics Assoc.,
1(12), 875-880.
Oteniya, L., Coles. R., Cowie, J. (2005). DemNet: A
Clinical Decision Support System to Aid the
Diagnosis of Dementia. In Proceedings of the
HealthCare Computing conference, Harrogate, U.K.,
289-297, March 2005.
Oteniya, L., Coles, R., Cowie, J. (2006). Constructing a
Bayesian belief network to support dementia diagnosis
using expert knowledge. In progress.
Werner, J.C., Fogarty, T. (2001). Genetic programming
applied to Collagen disease and thrombosis. In
Proceedings of The European Conference on
Principles and Practice of Knowledge Discovery in
Databases, 14-20, Germany.
Softwares: Netica Software, Norsys Software Corp.
DIAGNOSIS OF DEMENTIA AND ITS PATHOLOGIES USING BAYESIAN BELIEF NETWORKS
295
