
TOWARDS KNOWLEDGE-BASED INTEGRATION
OF PERSONAL HEALTH RECORD DATA FROM SENSORS
AND PATIENT OBSERVATIONS
John Puentes
Institut Telecom, Telecom Bretagne, Dpt. Image et Traitement de l’Information, Inserm U650 LaTIM, Brest, France
Jaakko Lähteenmäki
Knowledge Intensive Services, VTT Technical Research Center of Finland, Otaniemi, Finland
Keywords: Body monitoring, Personal health record, Physiological sensors, Heterogeneous data integration,
Knowledge model, Data understanding.
Abstract: Personal Health Records (PHR) containing physiological data collected by multiple sensors are being
increasingly used for wellness monitoring or disease management. These abundant complementary raw data
could be nevertheless disregarded given the challenges to understand and process it. We propose a
knowledge-based integration model of PHR data from sensors and personal observations, intended to
facilitate decision support in scenarios of cardiovascular disease monitoring. The model relates knowledge
at three data integration layers: elements identification, relations assessment, and refinement. Details on
specific elements of each layer are provided, along with a discussion of use and implementation guidelines.
1 INTRODUCTION
An increasing amount of physiological data
produced by multiple wearable body monitoring
devices, is gradually becoming available to
individuals (Jovanov et al., 2009). Depending on
user requirements - wellness monitoring or disease
management - these data streams can be either used
separately, or be stored with personal observations
in the Personal Health Record (PHR).
Whereas in wellness monitoring a particular
signal as weight or heart rate is periodically
measured and analyzed according to a goal, in
disease management several sensor inputs are
studied in order to continuously account for
abnormal parameters variation. The second scenario
implies significant additional work for the physician,
compelled to handle and interpret complementary
voluminous data, as well as for the patient asked to
acquire data on a regular basis. Such supplementary
common effort bears a major promise: both
physicians and patients expect a return in terms of
improved follow-up and decision support (DS).
Notwithstanding its importance, these data
acquired by body monitoring devices and personal
observations could be quickly neglected, given its
significant volume and the numerous challenges to
make sense out of it automatically (Garg et al.,
2010), unless it could be seamlessly integrated to the
PHR for further use after acquisition. This paper
defines and analyses a knowledge-based integration
model of PHR data from sensors and personal
observations, adapted to use cases of cardiovascular
disease. It focuses on the role of data for information
and knowledge discovery, by means of data
processing to provide pertinent DS (Figure 1).
We intend to explore the question of how to
combine relevant complementary data sources in the
PHR, enabling data utilization for DS, independently
of the concerned devices and data features. The
resulting integration model relies on a knowledge
infrastructure capable of handling meaningful
connections between sensors data, observations, and
information processing algorithms. It focuses
particularly on knowledge about sensors output,
annotations meaning, and related data structures.
Even though such integration is required in
various healthcare related contexts applications
(Kulkarni and Öztürk, 2007, Stuntebeck et al., 2008,
Martínez-López et al., 2008), it has not been
280
Puentes J. and Lähteenmäki J..
TOWARDS KNOWLEDGE-BASED INTEGRATION OF PERSONAL HEALTH RECORD DATA FROM SENSORS AND PATIENT OBSERVATIONS .
DOI: 10.5220/0003162502800285
In Proceedings of the International Conference on Health Informatics (HEALTHINF-2011), pages 280-285
ISBN: 978-989-8425-34-8
Copyright
c
2011 SCITEPRESS (Science and Technology Publications, Lda.)
addressed within a knowledge framework, to
facilitate conformity with multiple acquisition
devices, DS oriented data mining, and flexible user
queries. This work defines a knowledge-based
model to enable integrated PHR data understanding
and processing. In section 2, PHR functionality is
described, before presenting in section 3 the main
components of the knowledge-based model. Section
4 provides details on specific elements of each layer.
Section 5 discusses the use and implementation
guidelines of the proposed model. Section 6 presents
the conclusions.
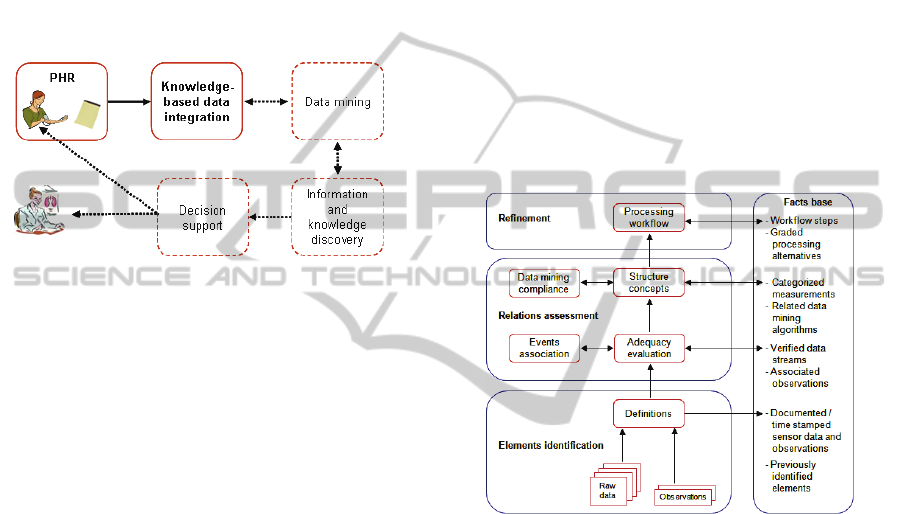
Figure 1: PHR knowledge-based data integration with
respect to subsequent data processing modules, as a means
to provide patient and physician DS.
2 PERSONAL HEALTH RECORD
DATA
As a complement to health care professionals
oriented Electronic Health Record (EHR), PHR
endorses individuals’ active role in their own
healthcare providing means to acquire, store, and
exchange health data like personal observations
related to specific events and physiological
measurements collected by sensors. Multiple
definitions as well as a variable range of complexity
characterize the approaches to build a functional
PHR (Tang et al., 2006). Furthermore, PHR has
been rarely incorporated to medical care flows, and
its adoption raises a wide variety of questions and
challenges (Halamka et al., 2008).
For our purpose, a PHR is mainly composed of
cardiovascular disease physiological sensor
measurements like activity, weight, temperature,
blood pressure, heart rate, and blood glucose, which
can be acquired by the patient throughout the day or
night, without the intervention of medical personnel,
as part of cardiovascular disease follow-up. The
PHR also contains personal observations related to
the occurrence of events like dizziness, weakness,
dyspnea, arrhythmias, or other anomalies, conveying
additional elements that properly documented have
the potential to reinforce DS. Supplementary data
like medications, laboratory tests, medical history,
and allergies that can be either accessed from the
patient EHR or copied from it to the PHR are not
taken into account for this analysis.
3 KNOWLEDGE-BASED DATA
INTEGRATION MODEL
Seamlessly DS requires data processing and
knowledge discovery to be absolutely independent
of available data resolution, imperfection,
heterogeneity, and formats. Besides, DS components
must be aware of the probable inadequacy of data
before activating the inference engine. Applying the
algorithms directly could produce severe errors.
Figure 2: Main components of the knowledge-based
model to integrate data from physiological sensors and
patient observations.
The conceptualized knowledge-based integration
of data from physiological sensors and observations
encompasses therefore (Figure 2): data definitions,
data structure concepts, association of reported
events with the sensors measurements, evaluation of
the obtained relations adequacy, verification of the
integrated data and relations compliance with data
mining requirements, and the respective workflow
generation. The model can be abstracted as the
interaction of three layers, i.e. elements
identification, relations assessment, and refinement.
3.1 Elements Identification
Raw data obtained from sensors e.g. vital signs,
blood glucose, or activity, are not likely to have the
same format, and even if the streams are
standardized the DS system still needs to properly
TOWARDS KNOWLEDGE-BASED INTEGRATION OF PERSONAL HEALTH RECORD DATA FROM SENSORS
AND PATIENT OBSERVATIONS
281

identify every pertinent element. This level contains
knowledge in the form of definitions making
possible to understand the: file format (XML, CSV,
text, binary, etc.), file source (sensor type,
constructor, and model), data structure (values
ordering, variables meaning, time stamps, and units),
and function to read the file. Equivalent separate
definitions permit to comprehend patient
observations. This kind of files is not generated by
the sensors, but created by the control application
running on the patient’s mobile phone or computer.
3.2 Relations Assessment
Once all the uploaded data streams elements have
been identified, events are associated and multiple
relations assessed. Data streams coherence is
examined looking for incomplete, invalid, or
contradictory measurements and observations that
could hinder subsequent processing, impeding as a
consequence to obtain proper DS. This step is
guided by knowledge about valid values, anomalies,
outliers, and accuracy criteria. Observations about
unusual events are added to the facts base according
to the corresponding time stamps.
Inference rules are then applied to define a DS-
oriented data structure. Compliance with related
predefined data mining algorithms is verified,
determining the valid data streams of available
previous and current measurements, depending on
DS requests. Knowledge at this stage mainly
categorizes measured values according to computed
characteristics. Additionally, common time intervals
of combined measurements are detected.
3.3 Refinement
Further detail about integrated data usability for
knowledge discovery, is defined by assembling the
appropriate processing workflow to answer a DS
query. Taking into account the categorized
measurements variability and the analysis goal
extent, the significance of intended processing
alternatives is graded against specific criteria. This
mechanism is necessary to produce a unified
workflow of processing steps, depending on the
quality of available data. The grading criteria
determine hence up to what point and how, the DS
request can be answered with validated data. To that
end, knowledge in the form of rules about
processing algorithms features linked to DS goals is
embedded in this layer.
4 MODEL ELEMENTS
Schematic descriptions of the three knowledge
layers components are presented in the next sections,
to illustrate how the different model elements are
interrelated.
4.1 Definitions
Basic reference knowledge about the observed
variables’ characteristics is stored in the first layer of
the model, permitting to have a global evaluation of
available data quality. The following definitions
were considered to initially assess a database:
Time reference to be used when analyzing the
integrated data – date, hour, minutes, and concerned
measurement sessions. It is taken as the starting
point in time to evaluate a group of measurement
sessions.
Time measurement definitions and related units –
instant and interval. Values can vary from a specific
moment, to intervals of minutes, hours, days, weeks,
or months.
Elements of a session - measurement, user and
session identification, date, start time, duration,
sensor, or observation report.
Activity definition and units – amount of steps
per time unit. It depends on the pedometer
characteristics and can be expressed in additional
terms like distance, speed, etc.
Pedometer model – brand, model, activity
definition, measured values ordering, accuracy, and
file type.
Blood pressure definition and units – systolic and
diastolic blood pressure measured at the upper arm
in mmHg.
Blood pressure meter model – brand, model,
blood pressure definition, measured values ordering,
accuracy, and file type.
Heart rate definition and units – pulse in beats
per second.
Heart rate monitor model – brand, model, heart
rate definition, measured values ordering, accuracy,
and file type.
Skin temperature measurement definition and
related units – heat in degree Celsius. It depends on
the thermometer characteristics and can be
expressed in other units.
Thermometer model – brand, model, temperature
definition, measured values ordering, accuracy, and
file type.
Weight measurement definition and units – sub-
HEALTHINF 2011 - International Conference on Health Informatics
282

ject’s body mass in kilograms and grams.
Scale model – brand, model, weight definition,
measured values ordering, accuracy, and file type.
Glucose measurement definition and related
units – sugar concentration in mmol/L or mg/dL.
Glucometer model – brand, model, glucose
measurement definition, values ordering, accuracy,
and file type.
Observations source description – source
application, time stamp, and file type.
Observations definition and description –
dizziness (confusion, loss of stability and
perception), weakness (discomfort, fatigue), dyspnea
(distress, breathlessness), quantified to levels such as
“none”, “occasionally” and “frequently”.
These definitions can be extended if more detailed
descriptions are used, based for instance on a
standard (IEEE Health Informatics, 2009).
4.2 Adequacy Evaluation
and Events Association
The second layer of the model contains knowledge
about relations and validations to be assessed, with
the objective of evaluating adequacy and data
mining compliance of the stored data streams. After
database elements identification, the following
relations are examined:
Time stamps during a measurement session can
be sequential or fragmented in continuous sub-
intervals. When the second case is detected a list of
sub-intervals is generated.
Valid steps counts - 0 to 180 steps per minute.
Anomalies in steps counts - negative values, time
slots without measurement, or long sequences of
constant values (except 0 steps).
Outliers in steps counts - more than 180 steps per
minute for a normal subject.
Valid blood pressure values - normal systolic
120/140 mmHg and normal diastolic 80/90 mmHg.
Anomalies of blood pressure values – lower
(systolic < 50 mmHg / diastolic < 35 mmHg), or
higher (systolic > 230 mmHg / diastolic > 140
mmHg) than physiological limits.
Outliers of blood pressure values – for systolic
between 150-230 mmHg, or 90-50 mmHg; for
diastolic between 100-140 mmHg, or between 70-35
mmHg.
Valid heart rate values - at rest 40-60 bpm (beats
per minute), in moderate activity 60-80 bpm,
walking 76-108 bpm, during exercise 109-160.
These magnitudes vary depending on age, weight,
height, and clinical condition.
Anomalies of heart rate values – lower than 40
bmp or higher than 160 bpm.
Outliers of heart rate values - punctual sets of
rather low or high bpm compared to the rest, within
a session.
Valid skin temperature values – from 10 to 40
C°.
Anomalies of skin temperature measurements -
continuous repeated changes from low to high
values (or inversely).
Outliers of temperature measurements -
continuous low or high temperatures periods.
Valid weight measurements – table of values
according to age, height, and clinical condition.
Anomalies of weight measurements - negative
values, very low or high values with respect to valid
measurements, or drastic changes.
Outliers of weight measurements – lower or
higher points than expected in a sequence.
Valid glucose measurements – 3.83 to 8.88
mmol/L, or 69 to 160 mg/dL.
Anomalies of glucose measurements - very low
or high punctual values.
Outliers in glucose measurements - continuous
low or high glucose periods.
Observation report content –
observations
definitions presented in section 4.1, rank on a scale
given by the patient to the sensation, circumstance
that provoked it, frequency, source application, and
comments.
Valid observation report. Applications to create
observations reports must comply with the required
observation report content.
Anomalies in observations. Although,
applications to create observations reports are
designed to prevent input errors, files can be
corrupted during transfer. Therefore, it is necessary
to verify all the parameters validity.
Outliers in observations. Depending on the
pathology and patient profile, some observations
could be considered as outliers because of the
severity, duration, frequency, and/or circumstances.
Those particular events need to be identified and
displayed separately.
Findings about verified data are stored in the facts
base to be used at the refinement stage.
TOWARDS KNOWLEDGE-BASED INTEGRATION OF PERSONAL HEALTH RECORD DATA FROM SENSORS
AND PATIENT OBSERVATIONS
283

4.3 Structure Concepts
and Data Mining Compliance
As part of the data exploration procedure, it is also
necessary to obtain additional information, about
available data sets compliance with the sought DS
request. The suggested list of knowledge
components is not exhaustive, because DS features
and processes are not examined in this work.
However, a basic scheme is proposed, in order to
illustrate how the model is expected to prepare a
structure of concepts. Some of these knowledge
components are:
Description of data streams depending on the
presence of outliers and abnormal measurements.
Statistical description of data streams. Multi-
parameter statistical description of the valid
measurements (continuous sequences or scattered
values of punctual values).
Common reference profiles. In several cases,
measurement patterns could appear. A set of rules
describes the reference profiles.
Characterization of data streams according to
differences with respect to pre-defined common
reference profiles.
Data distribution and grouping at different
degrees of temporal resolution. Identify data and
observations that correspond to adjustable time
intervals, from minutes to months.
Temporal reasoning. Temporal relations between
measurements and observations, focused on
simultaneity and sequencing.
Generate a global annotated description of the
examined data streams and observations.
At this point, it is possible to carry out an evaluation
to examine the compliance of available data with
pre-defined data mining algorithms, associated to the
respective DS request. Such evaluation verifies if the
global annotated description does not contain
penalizing facts, which will permit to conclude
before describing the processing workflow that
collected values are not reliable. For instance,
significant amount of anomalous values, outliers,
poor statistical descriptors, and/or incoherent
temporal relations, will prevent any further
processing.
4.4 Processing Workflow
When evaluated data complies with the algorithms
of a given DS request, the knowledge-based model
defines to which data sets those algorithms can be
applied. Again, the proposed list of knowledge
components is not exhaustive given its intrinsic
relation to the wanted DS:
Identification of candidate algorithms using a set
of rules.
Evaluation of the differences between
characteristics of expected input for each candidate
algorithms and available data.
Grading of the detected input differences
according to a significance scale.
Construction of a processing workflow list,
containing the ordered algorithms and associated
data sets.
Depending on the asked DS, some processing
workflows are likely to be more elaborated than
others. Thereafter the knowledge-based data
integration model output is applied by a procedural-
oriented system. Addition of other sensors like for
instance, oxygen saturation or respiratory rate, will
require expanding the elements of each knowledge
layer accordingly, as well as enlarged procedures to
integrate sensors data and observations.
5 DISCUSSION
The proposed model is a first attempt to integrate
data from multiple sensors and patient observations
at the acquisition and processing stages, by means of
a knowledge-based framework. It assumes that these
data are part of the PHR, easily accessed by patients
and clinical personnel alike, and is capable of
handling DS requests made by any of them. Answers
to those specific requests should be obtained
according to an optimal processing workflow
produced by the model, making use of pre-defined
algorithms and the relative significance of
longitudinal data.
It is important to note that data values are not
likely to be continuous, predictable or synchronized,
as in more conventional approaches like data
streaming management or the so-called wide-area
vigilance network (Han and Kamber, 2006). In our
particular case, the integration of asynchronous and
incomplete patient observations with partially
unreliable data from sensors, require to go beyond
separate data sources storage and database queries.
Furthermore, relevant information extraction
depends fundamentally on previously validated
knowledge, instead of blind processing routines.
Still, that knowledge base should evolve
dynamically, depending on the patient changing
condition, the respective variable volume of sensors
data, its quality, and the corresponding variable user
HEALTHINF 2011 - International Conference on Health Informatics
284

needs.
Different strategies could be applied to
implement the proposed knowledge-based model.
Some criteria for evaluating alternatives include
among others: easy representation of prior
knowledge statements, simple structure and
maintenance of facts bases, straightforward
definition of rules and reasoning mechanisms,
portability, interoperability of involved software
components, feasible scalable development, rich
data visualization resources, and web services
deployment. The decision may involve using
different specialized programming languages in
order to optimize specific modules, and in that case
the model implementation would be an embedded
engine of a larger distributed system.
Envisioned applications and services that could
make use of the proposed data integration model are
mainly related to wellness monitoring and disease
management. Given the richness of possible
integrated data analysis in these contexts, DS queries
must be controlled, precise, and constrained to
verified processing methods. For this reason,
available validated data sometimes may not be
relevant to answer a DS request, and the system
should be capable, thanks to the knowledge-based
model, to opportunely inform about such situation.
However, knowledge definitions are flexible enough
to be independently adapted at the three levels of the
model, and completed with other rules.
6 CONCLUSIONS
Regardless of the multiple ways to collect and
structure physiological sensors data and patient
observations, integration of these data for combined
analysis and interpretation requires embedded
knowledge at different levels. We formulated a
preliminary proposal towards the integration of
complex relationships between various physiological
sensors data and patient observations, in order to
produce goal oriented processing workflows. The
resulting knowledge-based data integration model is
intended to define how to process PHR data,
applying comprehensive dedicated knowledge
clusters, to validate goal oriented inferences. Further
work concerns the development and evaluation of a
complete prototype including clinical data from the
EHR, as well as the assessment of DS results for
specific use cases. Being an initial attempt to
formulate a general methodology, multiple open
questions remain beyond the conception of a
working system, like acceptance, performance, and
usability.
ACKNOWLEDGEMENTS
This work was supported in part by Telecom
Bretagne and in part by VTT and the Finnish
Funding Agency for Technology and Innovation
(Tekes) in the framework of the ITEA2/Care4Me
project.
REFERENCES
Garg, M. K., Kim, D-J., Turaga, D. S., Prabhakaran, B.,
2010. Multimodal analysis of body sensor network
data streams for real-time healthcare. In Proc. ACM
SIGMM International Conference on Multimedia
Information Retrieval, Philadelphia, USA, pp. 469-
478.
Halamka, J. D., Mandl, K. D., Tang, P. C., 2008. Early
experiences with personal health records. Journal of
the American Medical Informatics Association, vol.
15, no. 1, pp. 1-7.
Han, J., Kamber, M., 2006. Data Mining: Concepts and
Techniques. Morgan Kaufmann Series in Data
Management Systems, 2
nd
edition, pp. 467-488.
IEEE Health Informatics, 2009. Personal Health Device
Communication, Part 11073-10441: Device
Specialization - Cardiovascular Fitness and Activity
Monitor. IEEE Engineering in Medicine and Biology
Society, 11073™ Standard Committee, 85 pp.
Jovanov, E., Poon, C., Yang, G-Z., Zhang, Y. T., 2009.
Body sensor networks: from theory to emerging
applications. Guest Editorial. IEEE Transactions on
Information Technology in Biomedicine, vol. 13, no. 6,
pp. 859-863.
Kulkarni, P., Öztürk, Y., 2007. Requirements and design
spaces of mobile medical care. ACM SIGMOBILE
Mobile Computing and Communications Review, vol.
11, no. 3, pp. 12-30.
Martínez-López, R., Millán-Ruiz, D., Martín-Domínguez,
A., Toro-Escudero, M. A., 2008. An architecture for
next-generation of telecare systems using ontologies,
rules engines and data mining. In Proc. CIMCA,
IAWTIC, and ISE International Conferences, Vienna,
Austria, pp. 31-36.
Stuntebeck, E. P., Davis II, J. S., Abowd, G. D., Blount,
M., 2008. HealthSense: classification of health-related
sensor data through user-assisted machine learning. In
Proc. 9
th
workshop on Mobile Computing Systems and
Applications, Napa Valley, USA, pp.1-5.
Tang, P. C., Ash, J. S., Bates, D. W., Overhage, J. M.,
Sands, D. Z., 2006. Personal health records:
definitions, benefits, and strategies for overcoming
barriers to adoption. Journal of the American Medical
Informatics Association, vol. 13, no. 2, pp. 121-126.
TOWARDS KNOWLEDGE-BASED INTEGRATION OF PERSONAL HEALTH RECORD DATA FROM SENSORS
AND PATIENT OBSERVATIONS
285
